Health belief model
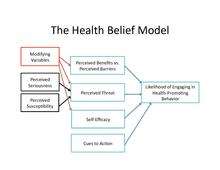
The health belief model (HBM) is a psychological health behavior change model developed to explain and predict health-related behaviors, particularly in regard to the uptake of health services.[1][2] The health belief model was developed in the 1950s by social psychologists at the U.S. Public Health Service[2][3] and remains one of the best known and most widely used theories in health behavior research.[4][5] The health belief model suggests that people's beliefs about health problems, perceived benefits of action and barriers to action, and self-efficacy explain engagement (or lack of engagement) in health-promoting behavior.[2][3] A stimulus, or cue to action, must also be present in order to trigger the health-promoting behavior.[2][3]
History
One of the first theories of health behavior,[5] the health belief model was developed in the 1950s by social psychologists Irwin M. Rosenstock, Godfrey M. Hochbaum, S. Stephen Kegeles, and Howard Leventhal at the U.S. Public Health Service to better understand the widespread failure of screening programs for tuberculosis.[4][6] The health belief model has been applied to predict a wide variety of health-related behaviors such as being screened for the early detection of asymptomatic diseases[2] and receiving immunizations.[2] More recently, the model has been applied to understand patients' responses to symptoms of disease,[2] compliance with medical regimens,[2] lifestyle behaviors (e.g., sexual risk behaviors),[6] and behaviors related to chronic illnesses,[2] which may require long-term behavior maintenance in addition to initial behavior change.[2] Amendments to the model were made as late as 1988 to incorporate emerging evidence within the field of psychology about the role of self-efficacy in decision-making and behavior.[5][6]
Theoretical constructs
The following constructs of the health belief model are proposed to vary between individuals and predict engagement in health-related behaviors (e.g., getting vaccinated, getting screened for asymptomatic diseases, exercising).[2]
| Health belief model chart (smoking as an example) | |||||||
|---|---|---|---|---|---|---|---|
| Modifying Variables
(age, gender, race, economy, characteristics) |
Perceived Severity
+ Perceived Susceptibility |
+ | perceived benefit
- perceived barriers |
+ | Cues to Action | = | taking action (or not) |
| (base score for this person's health) | (base score as to the belief that smoking will harm one's health) | (base score for smoking behavior) | |||||
Perceived severity
Perceived severity refers to the subjective assessment of the severity of a health problem and its potential consequences.[2][6] The health belief model proposes that individuals who perceive a given health problem as serious are more likely to engage in behaviors to prevent the health problem from occurring (or reduce its severity). Perceived seriousness encompasses beliefs about the disease itself (e.g., whether it is life-threatening or may cause disability or pain) as well as broader impacts of the disease on functioning in work and social roles.[2][3][6] For instance, an individual may perceive that influenza is not medically serious, but if he or she perceives that there would be serious financial consequences as a result of being absent from work for several days, then he or she may perceive influenza to be a particularly serious condition.
Perceived susceptibility
Perceived susceptibility refers to subjective assessment of risk of developing a health problem.[2][3][6] The health belief model predicts that individuals who perceive that they are susceptible to a particular health problem will engage in behaviors to reduce their risk of developing the health problem.[3] Individuals with low perceived susceptibility may deny that they are at risk for contracting a particular illness.[3] Others may acknowledge the possibility that they could develop the illness, but believe it is unlikely.[3] Individuals who believe they are at low risk of developing an illness are more likely to engage in unhealthy, or risky, behaviors. Individuals who perceive a high risk that they will be personally affected by a particular health problem are more likely to engage in behaviors to decrease their risk of developing the condition.
The combination of perceived severity and perceived susceptibility is referred to as perceived threat.[6] Perceived severity and perceived susceptibility to a given health condition depend on knowledge about the condition.[3] The health belief model predicts that higher perceived threat leads to higher likelihood of engagement in health-promoting behaviors.
Perceived benefits
Health-related behaviors are also influenced by the perceived benefits of taking action.[6] Perceived benefits refer to an individual's assessment of the value or efficacy of engaging in a health-promoting behavior to decrease risk of disease.[2] If an individual believes that a particular action will reduce susceptibility to a health problem or decrease its seriousness, then he or she is likely to engage in that behavior regardless of objective facts regarding the effectiveness of the action.[3] For example, individuals who believe that wearing sunscreen prevents skin cancer are more likely to wear sunscreen than individuals who believe that wearing sunscreen will not prevent the occurrence of skin cancer.
Perceived barriers
Health-related behaviors are also a function of perceived barriers to taking action.[6] Perceived barriers refer to an individual's assessment of the obstacles to behavior change.[2] Even if an individual perceives a health condition as threatening and believes that a particular action will effectively reduce the threat, barriers may prevent engagement in the health-promoting behavior. In other words, the perceived benefits must outweigh the perceived barriers in order for behavior change to occur.[2][6] Perceived barriers to taking action include the perceived inconvenience, expense, danger (e.g., side effects of a medical procedure) and discomfort (e.g., pain, emotional upset) involved in engaging in the behavior.[3] For instance, lack of access to affordable health care and the perception that a flu vaccine shot will cause significant pain may act as barriers to receiving the flu vaccine.
Modifying variables
Individual characteristics, including demographic, psychosocial, and structural variables, can affect perceptions (i.e., perceived seriousness, susceptibility, benefits, and barriers) of health-related behaviors.[3] Demographic variables include age, sex, race, ethnicity, and education, among others.[3][6] Psychosocial variables include personality, social class, and peer and reference group pressure, among others.[3] Structural variables include knowledge about a given disease and prior contact with the disease, among other factors.[3] The health belief model suggests that modifying variables affect health-related behaviors indirectly by affecting perceived seriousness, susceptibility, benefits, and barriers.[3][6]
Cues to action
The health belief model posits that a cue, or trigger, is necessary for prompting engagement in health-promoting behaviors.[2][3][4] Cues to action can be internal or external.[2][4] Physiological cues (e.g., pain, symptoms) are an example of internal cues to action.[2][6] External cues include events or information from close others,[2] the media,[4] or health care providers[2] promoting engagement in health-related behaviors. Examples of cues to action include a reminder postcard from a dentist, the illness of a friend or family member, and product health warning labels. The intensity of cues needed to prompt action varies between individuals by perceived susceptibility, seriousness, benefits, and barriers.[3] For example, individuals who believe they are at high risk for a serious illness and who have an established relationship with a primary care doctor may be easily persuaded to get screened for the illness after seeing a public service announcement, whereas individuals who believe they are at low risk for the same illness and also do not have reliable access to health care may require more intense external cues in order to get screened.
Self-efficacy
Self-efficacy was added to the four components of the health belief model (i.e., perceived susceptibility, seriousness, benefits, and barriers) in 1988.[6][7] Self-efficacy refers to an individual's perception of his or her competence to successfully perform a behavior.[6] Self-efficacy was added to the health belief model in an attempt to better explain individual differences in health behaviors.[7] The model was originally developed in order to explain engagement in one-time health-related behaviors such as being screened for cancer or receiving an immunization.[3][7] Eventually, the health belief model was applied to more substantial, long-term behavior change such as diet modification, exercise, and smoking.[7] Developers of the model recognized that confidence in one's ability to effect change in outcomes (i.e., self-efficacy) was a key component of health behavior change.[6][7]
Empirical support
The health belief model has gained substantial empirical support since its development in the 1950s.[2][4] It remains one of the most widely used and well-tested models for explaining and predicting health-related behavior.[4] A 1984 review of 18 prospective and 28 retrospective studies suggests that the evidence for each component of the health belief model is strong.[2] The review reports that empirical support for the health belief model is particularly notable given the diverse populations, health conditions, and health-related behaviors examined and the various study designs and assessment strategies used to evaluate the model.[2] A more recent meta-analysis found strong support for perceived benefits and perceived barriers predicting health-related behaviors, but weak evidence for the predictive power of perceived seriousness and perceived susceptibility.[4] The authors of the meta-analysis suggest that examination of potential moderated and mediated relationships between components of the model is warranted.[4]
Applications
The health belief model has been used to develop effective interventions to change health-related behaviors by targeting various aspects of the model's key constructs.[4][7] Interventions based on the health belief model may aim to increase perceived susceptibility to and perceived seriousness of a health condition by providing education about prevalence and incidence of disease, individualized estimates of risk, and information about the consequences of disease (e.g., medical, financial, and social consequences).[6] Interventions may also aim to alter the cost-benefit analysis of engaging in a health-promoting behavior (i.e., increasing perceived benefits and decreasing perceived barriers) by providing information about the efficacy of various behaviors to reduce risk of disease, identifying common perceived barriers, providing incentives to engage in health-promoting behaviors, and engaging social support or other resources to encourage health-promoting behaviors.[6] Furthermore, interventions based on the health belief model may provide cues to action to remind and encourage individuals to engage in health-promoting behaviors.[6] Interventions may also aim to boost self-efficacy by providing training in specific health-promoting behaviors,[6][7] particularly for complex lifestyle changes (e.g., changing diet or physical activity, adhering to a complicated medication regimen).[7] Interventions can be aimed at the individual level (i.e., working one-on-one with individuals to increase engagement in health-related behaviors) or the societal level (e.g., through legislation, changes to the physical environment).[8]
Limitations
The health belief model attempts to predict health-related behaviors by accounting for individual differences in beliefs and attitudes.[2] However, it does not account for other factors that influence health behaviors.[2] For instance, habitual health-related behaviors (e.g., smoking, seatbelt buckling) may become relatively independent of conscious health-related decision making processes.[2] Additionally, individuals engage in some health-related behaviors for reasons unrelated to health (e.g., exercising for aesthetic reasons).[2] Environmental factors outside an individual's control may prevent engagement in desired behaviors.[2] For example, an individual living in a dangerous neighborhood may be unable to go for a jog outdoors due to safety concerns. Furthermore, the health belief model does not consider the impact of emotions on health-related behavior.[6] Evidence suggests that fear may be a key factor in predicting health-related behavior.[6]
The theoretical constructs that constitute the health belief model are broadly defined.[4] Furthermore, the health belief model does not specify how constructs of the model interact with one another.[4][6] Therefore, different operationalizations of the theoretical constructs may not be strictly comparable across studies.[6][9]
Research assessing the contribution of cues to action in predicting health-related behaviors is limited.[2][3][4][6] Cues to action are often difficult to assess, limiting research in this area.[3][6] For instance, individuals may not accurately report cues that prompted behavior change.[3] Cues such as a public service announcement on television or on a billboard may be fleeting and individuals may not be aware of their significance in prompting them to engage in a health-related behavior.[3][6] Interpersonal influences are also particularly difficult to measure as cues.[3]
References
- ↑ Siddiqui TR, Ghazal S, Bibi S, Ahmed W, Sajjad SF (2016) Use of the Health Belief Model for the Assessment of Public Knowledge and Household Preventive Practices in Karachi, Pakistan, a Dengue-Endemic City. PLOS Neglected Tropical Diseases 10(11): e0005129. doi: 10.1371/journal.pntd.0005129
- 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 Janz, Nancy K.; Marshall H. Becker (1984). "The Health Belief Model: A Decade Later". Health Education & Behavior. 11 (1): 1–47. doi:10.1177/109019818401100101.
- 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 Rosenstock, Irwin (1974). "Historical Origins of the Health Belief Model". Health Education & Behavior. 2 (4): 328–335. doi:10.1177/109019817400200403.
- 1 2 3 4 5 6 7 8 9 10 11 12 13 Carpenter, Christopher J. (2010). "A meta-analysis of the effectiveness of health belief model variables in predicting behavior". Health Communication. 25 (8): 661–669. doi:10.1080/10410236.2010.521906.
- 1 2 3 Glanz, Karen; Bishop, Donald B. (2010). "The role of behavioral science theory in development and implementation of public health interventions". Annual Review of Public Health. 31: 399–418. doi:10.1146/annurev.publhealth.012809.103604.
- 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 Glanz, Karen; Barbara K. Rimer; K. Viswanath (2008). Health behavior and health education: theory, research, and practice. (PDF) (4th ed.). San Francisco, CA: Jossey-Bass. pp. 45–51. ISBN 978-0787996147.
- 1 2 3 4 5 6 7 8 Rosenstock, Irwin M.; Strecher, Victor J.; Becker, Marshall H. (1988). "Social learning theory and the health belief model". Health Education & Behavior. 15 (2): 175–183. doi:10.1177/109019818801500203.
- ↑ Stretcher, Victor J.; Irwin M. Rosenstock (1997). "The health belief model". In Andrew Baum. Cambridge handbook of psychology, health and medicine. Cambridge, UK: Cambridge University Press. pp. 113–117. ISBN 0521430739.
- ↑ Maiman, Lois A.; Marshall H. Becker; John P. Kirscht; Don P. Haefner; Robert H. Drachman (1977). "Scales for Measuring Health Belief Model Dimensions: A Test of Predictive Value, Internal Consistency, and Relationships Among Beliefs" (PDF). Health Education & Behavior. 5: 215–230. doi:10.1177/109019817700500303. Retrieved 2013-11-22.