Erythropoietin
Erythropoietin (EPO), also known as hematopoietin or hemopoietin, is a glycoprotein that controls erythropoiesis, or red blood cell production. It is a cytokine (protein signaling molecule) for erythrocyte (red blood cell) precursors in the bone marrow. Human EPO has a molecular weight of 34 kDa.
Erythropoietin is produced by interstitial fibroblasts in the kidney in close association with peritubular capillary and proximal convoluted tubule. It is also produced in perisinusoidal cells in the liver. While liver production predominates in the fetal and perinatal period, renal production is predominant during adulthood. It is pronounced (/ɪˌrɪθroʊˈpɔɪɪtən/ or /ɪˌrɪθroʊpoʊˈɛtɪn, -rə-, -ˈiː-, -tən/.[3][4][5])
Exogenous erythropoietin can be provided to people whose kidneys cannot make enough. Recombinant human erythropoietin (rhEPO) is produced by recombinant DNA technology in cell culture. Several different pharmaceutical agents are available with a variety of glycosylation patterns and are collectively called erythropoiesis-stimulating agents (ESA). Major examples are epoetin alfa and epoetin beta. The specific details for labeled use vary between the package inserts, but ESAs have been used in the treatment of anemia in chronic kidney disease, anemia in myelodysplasia, and in anemia from cancer chemotherapy. Boxed warnings include a risk of death, myocardial infarction, stroke, venous thromboembolism, and tumor recurrence.[6] rhEPO has been used illicitly as a performance-enhancing drug;[7] it can often be detected in blood, due to slight differences from the endogenous protein, for example, in features of posttranslational modification.
Function
Red blood cell production
Erythropoietin is an essential hormone for red blood cell production. Without it, definitive erythropoiesis does not take place. Under hypoxic conditions, the kidney will produce and secrete erythropoietin to increase the production of red blood cells by targeting CFU-E, proerythroblast and basophilic erythroblast subsets in the differentiation. Erythropoietin has its primary effect on red blood cell progenitors and precursors (which are found in the bone marrow in humans) by promoting their survival through protecting these cells from apoptosis, or cell death.
Erythropoietin is the primary erythropoietic factor that cooperates with various other growth factors (e.g., IL-3, IL-6, glucocorticoids, and SCF) involved in the development of erythroid lineage from multipotent progenitors. The burst-forming unit-erythroid (BFU-E) cells start erythropoietin receptor expression and are sensitive to erythropoietin. Subsequent stage, the colony-forming unit-erythroid (CFU-E), expresses maximal erythropoietin receptor density and is completely dependent on erythropoietin for further differentiation. Precursors of red cells, the proerythroblasts and basophilic erythroblasts also express erythropoietin receptor and are therefore affected by it.
Nonhematopoietic roles
Erythropoietin was reported to have a range of actions beyond stimulation of erythropoiesis including vasoconstriction-dependent hypertension, stimulating angiogenesis, and promoting cell survival via activation of Epo receptors resulting in anti-apoptotic effects on ischemic tissues. However this proposal is controversial with numerous studies showing no effect.[8] It is also inconsistent with the low levels of Epo receptors on those cells. Clinical trials in humans with ischemic heart, neural and renal tissues have not demonstrated the same benefits seen in animals. In addition some research studies have shown its neuroprotective effect on diabetic neuropathy, however these data were not confirmed in clinical trials that have been conducted on the deep peroneal, superficial peroneal, tibial and sural nerves.[9]
Mechanism of action
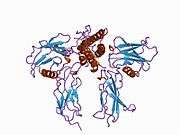
Erythropoietin has been shown to exert its effects by binding to the erythropoietin receptor (EpoR).[10][11]
EPO is highly glycosylated (40% of total molecular weight), with half-life in blood around five hours. EPO's half-life may vary between endogenous and various recombinant versions. Additional glycosylation or other alterations of EPO via recombinant technology have led to the increase of EPO's stability in blood (thus requiring less frequent injections). EPO binds to the erythropoietin receptor on the red cell progenitor surface and activates a JAK2 signaling cascade. This initiates the STAT5, PIK3 and Ras MAPK pathways. This results in differentiation, survival and proliferation of the erythroid cell.[12] SOCS1, SOCS3 and CIS are also expressed which act as negative regulators of the cytokine signal.[13] High level erythropoietin receptor expression is localized to erythroid progenitor cells. While there are reports that EPO receptors are found in a number of other tissues, such as heart, muscle, kidney and peripheral/central nervous tissue, those results are confounded by nonspecificity of reagents such as anti-EpoR antibodies. In controlled experiments, EPO receptor is not detected in those tissues. In the bloodstream, red cells themselves do not express erythropoietin receptor, so cannot respond to EPO. However, indirect dependence of red cell longevity in the blood on plasma erythropoietin levels has been reported, a process termed neocytolysis.
Synthesis and regulation
Erythropoietin levels in blood are quite low in the absence of anemia, at around 10 mU/ml. However, in hypoxic stress, EPO production may increase up to 1000-fold, reaching 10,000 mU/ml of blood. In adults, EPO is synthesized mainly by interstitial cells in the peritubular capillary bed of the renal cortex, with additional amounts being produced in the liver,[14][15][16] and the pericytes in the brain.[17] Regulation is believed to rely on a feedback mechanism measuring blood oxygenation and iron availability.[18] Constitutively synthesized transcription factors for EPO, known as hypoxia-inducible factors, are hydroxylated and proteosomally digested in the presence of oxygen and iron. During normoxia GATA2 inhibits the promoter region for EPO. GATA2 levels decrease during hypoxia and allow the promotion of EPO production.[19]
Medical uses
Erythropoietins available for use as therapeutic agents are produced by recombinant DNA technology in cell culture, and include Epogen/Procrit (epoetin alfa) and Aranesp (darbepoetin alfa); they are used in treating anemia resulting from chronic kidney disease, chemotherapy induced anemia in patients with cancer, inflammatory bowel disease (Crohn's disease and ulcerative colitis)[20] and myelodysplasia from the treatment of cancer (chemotherapy and radiation). The package inserts include boxed warnings of increased risk of death, myocardial infarction, stroke, venous thromboembolism, and tumor recurrence, particularly when used to increase the hemoglobin levels to more than 11 to 12 g/dl.[6]
History
In 1905, Paul Carnot, a professor of medicine in Paris, and his assistant, Clotilde Deflandre, proposed the idea that hormones regulate the production of red blood cells. After conducting experiments on rabbits subject to bloodletting, Carnot and Deflandre attributed an increase in red blood cells in rabbit subjects to a hemotropic factor called hemopoietin. Eva Bonsdorff and Eeva Jalavisto continued to study red cell production and later called the hemopoietic substance 'erythropoietin'. Further studies investigating the existence of EPO by K.R. Reissman and Allan J. Erslev (Thomas Jefferson Medical College) demonstrated that a certain substance, circulated in the blood, is able to stimulate red blood cell production and increase hematocrit. This substance was finally purified and confirmed as erythropoietin, opening doors to therapeutic uses for EPO in diseases such as anemia.[18][21]
Hematologist John Adamson and nephrologist Joseph W. Eschbach looked at various forms of renal failure and the role of the natural hormone EPO in the formation of red blood cells. Studying sheep and other animals in the 1970s, the two scientists helped establish that EPO stimulates the production of red cells in bone marrow and could lead to a treatment for anemia in humans. In 1968, Goldwasser and Kung began work to purify human EPO, and managed to purify milligram quantities of over 95% pure material by 1977.[22] Pure EPO allowed the amino acid sequence to be partially identified and the gene to be isolated.[18] Later, a researcher at Columbia University discovered a way to synthesize EPO. Columbia University patented the technique and licensed it to Amgen.
In the 1980s, Adamson, Joseph W. Eschbach, Joan C. Egrie, Michael R. Downing and Jeffrey K. Browne conducted a clinical trial at the Northwest Kidney Centers for a synthetic form of the hormone, Epogen, produced by Amgen. The trial was successful, and the results were published in the New England Journal of Medicine in January 1987.[23]
In 1985, Lin et al isolated the human erythropoietin gene from a genomic phage library and were able to characterize it for research and production.[24] Their research demonstrated the gene for erythropoietin encoded the production of EPO in mammalian cells that is biologically active in vitro and in vivo. The commercial production of recombinant human erythropoietin (rhEpo) for treating anemia patients would begin soon after.
In 1989, the US Food and Drug Administration approved the hormone Epogen, which remains in use today.[25]
See also
References
- ↑ "Human PubMed Reference:".
- ↑ "Mouse PubMed Reference:".
- ↑ "Erythropoietin". Merriam-Webster Dictionary.
- ↑ "Erythropoietin". Dictionary.com Unabridged. Random House.
- ↑ "erythropoietin – definition of erythropoietin in English from the Oxford dictionary". OxfordDictionaries.com. Retrieved 2016-01-20.
- 1 2 "Safety Labeling Changes: Epogen/Procrit (epoetin alfa) and Aranesp (darbepoetin alfa)". MedWatch: The FDA Safety Information and Adverse Event Reporting Program. United States Food and Drug Administration. August 11, 2011.
- ↑ Momaya A, Fawal M, Estes R (April 2015). "Performance-enhancing substances in sports: a review of the literature". Sports Med. 45 (4): 517–531. PMID 25663250. doi:10.1007/s40279-015-0308-9.
- ↑ Elliott S, Sinclair AM (2012). "The effect of erythropoietin on normal and neoplastic cells". Biologics. 6: 163–89. PMC 3402043
 . PMID 22848149. doi:10.2147/BTT.S32281.
. PMID 22848149. doi:10.2147/BTT.S32281. - ↑ Hosseini-Zare MS, Dashti-Khavidaki S, Mahdavi-Mazdeh M, Ahmadi F, Akrami S (2012). "Peripheral neuropathy response to erythropoietin in type 2 diabetic patients with mild to moderate renal failure". Clinical Neurology and Neurosurgery. 114 (6): 663–7. PMID 22296650. doi:10.1016/j.clineuro.2012.01.007.
- ↑ Middleton SA, Barbone FP, Johnson DL, Thurmond RL, You Y, McMahon FJ, Jin R, Livnah O, Tullai J, Farrell FX, Goldsmith MA, Wilson IA, Jolliffe LK (1999). "Shared and unique determinants of the erythropoietin (EPO) receptor are important for binding EPO and EPO mimetic peptide". The Journal of Biological Chemistry. 274 (20): 14163–9. PMID 10318834. doi:10.1074/jbc.274.20.14163.
- ↑ Livnah O, Johnson DL, Stura EA, Farrell FX, Barbone FP, You Y, Liu KD, Goldsmith MA, He W, Krause CD, Pestka S, Jolliffe LK, Wilson IA (1998). "An antagonist peptide-EPO receptor complex suggests that receptor dimerization is not sufficient for activation". Nature Structural Biology. 5 (11): 993–1004. PMID 9808045. doi:10.1038/2965.
- ↑ Thomson, Angus W.; Lotze, Michael T. (2003-04-22). The Cytokine Handbook, Two-Volume Set. Gulf Professional Publishing. ISBN 9780080518794.
- ↑ Hodges, Vivien M.; Rainey, Susan; Lappin, Terence R.; Maxwell, A. Peter (2007-11-01). "Pathophysiology of anemia and erythrocytosis". Critical Reviews in Oncology/Hematology. 64 (2): 139–158. ISSN 1040-8428. PMID 17656101. doi:10.1016/j.critrevonc.2007.06.006.
- ↑ Jacobson LO, Goldwasser E, Fried W, Plzak L (1957). "Role of the kidney in erythropoiesis". Nature. 179 (4560): 633–4. PMID 13418752. doi:10.1038/179633a0.
- ↑ Fisher JW, Koury S, Ducey T, Mendel S (1996). "Erythropoietin production by interstitial cells of hypoxic monkey kidneys". British Journal of Haematology. 95 (1): 27–32. PMID 8857934. doi:10.1046/j.1365-2141.1996.d01-1864.x.
- ↑ Barrett, Kim E.; Barman, Susan M.; Boitano, Scott; Brooks, Heddwen (eds.). Ganong's review of Medical Physiology (24th ed.). McGraw Hill. p. 709. ISBN 978-1-25-902753-6.
- ↑ Ji, P. (24 November 2016). "Pericytes: new EPO-producing cells in the brain". Blood. 128 (21): 2483–2485. doi:10.1182/blood-2016-10-743880.
- 1 2 3 Jelkmann W (2007). "Erythropoietin after a century of research: younger than ever". European Journal of Haematology. 78 (3): 183–205. PMID 17253966. doi:10.1111/j.1600-0609.2007.00818.x.
- ↑ Jelkmann, W., 2011. Regulation of erythropoietin production. The Journal of physiology, 589(6), pp.1251-1258.
- ↑ Liu S, Ren J, Hong Z, Yan D, Gu G, Han G, Wang G, Ren H, Chen J, Li J (2013). "Efficacy of erythropoietin combined with enteral nutrition for the treatment of anemia in Crohn's disease: a prospective cohort study". Nutrition in Clinical Practice. 28 (1): 120–7. PMID 23064018. doi:10.1177/0884533612462744.
- ↑ Höke A (2005). Erythropoietin and the Nervous System. Berlin: Springer. ISBN 0-387-30010-4. OCLC 64571745.
- ↑ Miyake T, Kung CK, Goldwasser E (1977). "Purification of human erythropoietin". The Journal of Biological Chemistry. 252 (15): 5558–64. PMID 18467.
- ↑ Eschbach JW, Egrie JC, Downing MR, Browne JK, Adamson JW (1987). "Correction of the anemia of end-stage renal disease with recombinant human erythropoietin. Results of a combined phase I and II clinical trial". The New England Journal of Medicine. 316 (2): 73–8. PMID 3537801. doi:10.1056/NEJM198701083160203.
- ↑ Lin FK, Suggs S, Lin CH, Browne JK, Smalling R, Egrie JC, Chen KK, Fox GM, Martin F, Stabinsky Z (1985). "Cloning and expression of the human erythropoietin gene". Proceedings of the National Academy of Sciences of the United States of America. 82 (22): 7580–4. PMC 391376
 . PMID 3865178. doi:10.1073/pnas.82.22.7580.
. PMID 3865178. doi:10.1073/pnas.82.22.7580. - ↑ "Epogen Prescribing Information" (PDF).
Further reading
- Takeuchi M, Kobata A (1991). "Structures and functional roles of the sugar chains of human erythropoietins". Glycobiology. 1 (4): 337–46. PMID 1820196. doi:10.1093/glycob/1.4.337.
- Semba RD, Juul SE (2002). "Erythropoietin in human milk: physiology and role in infant health". Journal of Human Lactation. 18 (3): 252–61. PMID 12192960. doi:10.1177/089033440201800307.
- Ratcliffe PJ (2002). "From erythropoietin to oxygen: hypoxia-inducible factor hydroxylases and the hypoxia signal pathway". Blood Purification. 20 (5): 445–50. PMID 12207089. doi:10.1159/000065201.
- Westenfelder C (2002). "Unexpected renal actions of erythropoietin". Experimental Nephrology. 10 (5-6): 294–8. PMID 12381912. doi:10.1159/000065304.
- Becerra SP, Amaral J (2002). "Erythropoietin--an endogenous retinal survival factor". The New England Journal of Medicine. 347 (24): 1968–70. PMID 12477950. doi:10.1056/NEJMcibr022629.
- Genc S, Koroglu TF, Genc K (2004). "Erythropoietin and the nervous system". Brain Research. 1000 (1-2): 19–31. PMID 15053948. doi:10.1016/j.brainres.2003.12.037.
- Fandrey J (2004). "Oxygen-dependent and tissue-specific regulation of erythropoietin gene expression". American Journal of Physiology. Regulatory, Integrative and Comparative Physiology. 286 (6): R977–88. PMID 15142852. doi:10.1152/ajpregu.00577.2003.
- Juul S (2004). "Recombinant erythropoietin as a neuroprotective treatment: in vitro and in vivo models". Clinics in Perinatology. 31 (1): 129–42. PMID 15183662. doi:10.1016/j.clp.2004.03.004.
- Buemi M, Caccamo C, Nostro L, Cavallaro E, Floccari F, Grasso G (2005). "Brain and cancer: the protective role of erythropoietin". Medicinal Research Reviews. 25 (2): 245–59. PMID 15389732. doi:10.1002/med.20012.
- Sytkowski AJ (2007). "Does erythropoietin have a dark side? Epo signaling and cancer cells". Science's STKE. 2007 (395): pe38. PMID 17636183. doi:10.1126/stke.3952007pe38.
- Goldwasser, Eugene (2011). A Bloody Long Journey: Erythropoietin and the Person Who Isolated It. Xlibris. ISBN 978-1-4568-5737-0.
External links
- NYT – 1987 announcement of Epogen's clinical success
- Dynepo EPAR (European Public Assessment Report), PDF format, credit European Medicines Agency