Salivary gland neoplasm
| Salivary gland cancer | |
|---|---|
 The major salivary glands: the parotid gland (1), where most salivary gland tumors form, the submandibular gland (2), and the sublingual gland (3). | |
| Classification and external resources | |
| Specialty | Oncology |
| ICD-10 | C07-C08, D11 |
| ICD-9-CM | 142, 210.2 |
| MedlinePlus | 001040 |
| MeSH | D012468 |
Salivary gland cancer is a cancer that forms in tissues of a salivary gland. The salivary glands are classified as major and minor. The major salivary glands consist of the parotid, submandibular, and sublingual glands. The minor glands include small mucus-secreting glands located throughout the palate, nasal and oral cavity.[1] Salivary gland cancer is rare, with 2% of head and neck tumors forming in the salivary glands, the majority in the parotid.[2]
Classification
Due to diverse nature of salivary gland neoplasms, many different terms and classification systems have been used. Perhaps the most widely used currently is that system proposed by the World Health Organization in 2004, which classifies salivary neoplasms as primary or secondary, benign or malignant, and also by tissue of origin. This system defines five broad categories of salivary gland neoplasms:[3][4]
- Malignant epithelial tumors
- Acinic cell carcinoma
- Mucoepidermoid carcinoma
- Adenoid cystic carcinoma
- Polymorphous low-grade adenocarcinoma
- Epithelial-myoepithelial carcinoma
- Clear cell carcinoma, not otherwise specified
- Basal cell adenocarcinoma
- Sebaceous carcinoma
- Sebaceous lymphadenocarcinoma
- Cystadenocarcinoma
- Low-grade cribriform cystadenocarcinoma
- Mucinous adenocarcinoma
- Oncocytic carcinoma
- Salivary duct carcinoma
- Salivary duct carcinoma, not otherwise specified
- Adenocarcinoma, not otherwise specified
- Myoepithelial carcinoma
- Carcinoma ex pleomorphic adenoma
- Carcinosarcoma
- Metastasizing pleomorphic adenoma
- Squamous cell carcinoma
- Large cell carcinoma
- Lymphoepithelial carcinoma
- Sialoblastoma
- Benign epithelial tumors
- Pleomorphic adenoma
- Myoepithelioma
- Basal cell adenoma
- Warthin's tumor
- Oncocytoma
- Canalicular adenoma
- Lymphadenoma
- Sebaceous lymphadenoma
- Nonsebaceous lymphadenoma
- Ductal papilloma
- Inverted ductal papilloma
- Intraductal papilloma
- Sialadenoma papilliferum
- Cystadenoma
- Soft tissue tumors
- Hematolymphoid tumors
- Secondary tumors (i.e. a tumor which has metastasized to the salivary gland from a distant location)
Others, not included in the WHO classification above, include:[3]
- Intraosseous (central) salivary gland tumors
- Hybrid tumors (i.e. a tumor displaying combined forms of histologic tumor types)
- Hybrid carcinoma
- Others
- Others
- Keratocystoma
- Sialolipoma
Signs and symptoms
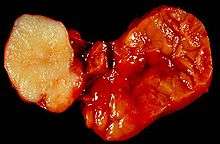
Signs include fluid draining from the ear, pain, numbness, weakness, trouble swallowing, and a lump. The most common symptom of major salivary gland cancer is a painless lump in the affected gland, sometimes accompanied by paralysis of the facial nerve.
Causes
The chief risk factor is chewing tobacco, followed by smoking. Other risk factors include older age, radiation therapy treatment to head or neck, and being exposed to certain carcinogenic substances at work.
Diagnosis
In most cases, local excision with a margin of normal tissue is the appropriate form of biopsy for a major salivary gland tumor. In the parotid region, this requires identification of the facial nerve. For submandibular tumors, the entire submandibular triangle is cleared. In contrast, minor salivary gland tumors have a higher likelihood of being malignant, and an incisional biopsy is performed initially so that definitive treatment can be planned. In the parotid region, the presence of pain, recent rapid enlargement of a preexisting nodule, skin involvement, or facial nerve paralysis suggests cancer. Enlarged cervical lymph nodes in association with a salivary gland tumor are considered a manifestation of cancer until proved otherwise. Fine-needle aspiration is indicated if accurate diagnosis will allow for better treatment planning.
Prevention
Abstaining from smoking, chewing tobacco. Maintaining a diet high in fiber and green leafy vegetables. Change your toothbrush at regular intervals (weekly)
Treatment
Treatment may include the following:
- Surgery with or without radiation
- Radiotherapy
Fast neutron therapy has been used successfully to treat salivary gland tumors,[5] and has shown to be significantly more effective than photons in studies treating unresectable salivary gland tumors.[6][7]*Chemotherapy.
History
Former San Diego Padres player Tony Gwynn died from this.
He was 54.
See also
References
- ↑ Shah JP; Patel SG (2001). Cancer of the Head and Neck. PMPH-USA. p. 240. ISBN 978-1-55009-084-0.
- ↑ Harari PM; Connor NP; Cai Grau (12 June 2009). Functional Preservation and Quality of Life in Head and Neck Radiotherapy. Springer Science & Business Media. p. 89. ISBN 978-3-540-73232-7.
- 1 2 Barnes L (23 December 2008). Surgical Pathology of the Head and Neck 1 (3rd ed.). Taylor & Francis. p. 511. ISBN 978-0-8493-9023-4.
- ↑ Barnes L (2005). "Chapter 5: Tumors of the salivary glands (chapter authors: Eveson JW, Auclair P, Gnepp DR, El-Naggar AK)". Pathology and Genetics of Head and Neck Tumours (PDF). International Agency for Research on Cancer, World Health Organization. p. 210. ISBN 978-92-832-2417-4.
- ↑ Douglas JD, Koh WJ , Austin-Seymour, M, Laramore GE. Treatment of Salivary Gland Neoplasms with fast neutron Radiotherapy. Arch Otolaryngol Head Neck Surg Vol 129 944-948 Sep 2003
- ↑ Laramore GE, Krall JM, Griffin TW, Duncan W, Richter MP, Saroja KR, Maor MH, Davis LW. Neutron versus photon irradiation for unresectable salivary gland tumors: final report of an RTOG-MRC randomized clinical trial. Int J Radiat Oncol Biol Phys. 1993 Sep 30;27(2):235-40.
- ↑ Krüll A, Schwarz R, Engenhart R, et al.: European results in neutron therapy of malignant salivary gland tumors. Bull Cancer Radiother 83 (Suppl): 125-9s, 1996
| ||||||||||||||||||||||||||
External links
- Salivary gland cancer entry in the public domain NCI Dictionary of Cancer Terms
- Clinically reviewed salivary gland cancer for patients from Cancer Research UK.
![]() This article incorporates public domain material from the U.S. National Cancer Institute document "Dictionary of Cancer Terms".
This article incorporates public domain material from the U.S. National Cancer Institute document "Dictionary of Cancer Terms".