Chancroid
| Chancroid | |
|---|---|
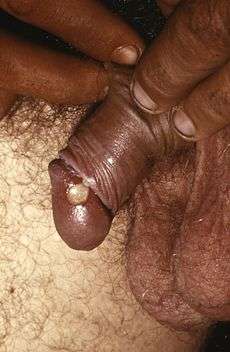 A chancroid lesion on penis | |
| Classification and external resources | |
| Specialty | Infectious disease |
| ICD-10 | A57 |
| ICD-9-CM | 099.0 |
| DiseasesDB | 5563 |
| MedlinePlus | 000635 |
| eMedicine | emerg/95 |
| MeSH | D002602 |
Chancroid (also known as soft chancre[1] and ulcus molle[2]) is a bacterial sexually transmitted infection characterized by painful sores on the genitalia. Chancroid is known to spread from one individual to another solely through sexual contact.
Causes
Chancroid is a bacterial infection caused by the fastidious Gram-negative streptobacillus Haemophilus ducreyi. It is a disease found primarily in developing countries, most prevalent in low socioeconomic groups, associated with commercial sex workers. In the United States socioeconomic status has not been found to be a factor in the spread of sexually transmitted diseases. [3]
Chancroid, caused by H. ducreyi has infrequently been associated with cases of Genital Ulcer Disease in the US, but has been isolated in up to 10% of genital ulcers diagnosed from STD clinics in Memphis and Chicago. [4]
Infection levels are very low in the Western world, typically around one case per two million of the population (Canada, France, Australia, UK and US). Most individuals diagnosed with chancroid have visited countries or areas where the disease is known to occur frequently, although outbreaks have been observed in association with crack cocaine use and prostitution.
Chancroid is a risk factor for contracting HIV, due to their ecological association or shared risk of exposure, and biologically facilitated transmission of one infection by the other.
Pathogenesis
H. ducreyi enters skin through microabrasions incurred during sexual intercourse. A local tissue reaction leads to development of erythomatous papule, which progresses to pustule in 4–7 days. It then undergoes central necrosis to ulcerate.[5]
Signs and symptoms
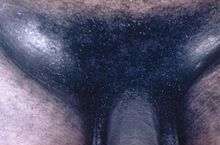
These are only local and no systemic manifestations are present.[6] The ulcer characteristically:
- Ranges in size dramatically from 3 to 50 mm (1/8 inch to two inches) across
- Is painful
- Has sharply defined, undermined borders
- Has irregular or ragged borders
- Has a base that is covered with a gray or yellowish-gray material
- Has a base that bleeds easily if traumatized or scraped
- painful lymphadenopathy occurs in 30 to 60% of patients.
- dysuria (pain with urination) and dyspareunia (pain with intercourse) in females
About half of infected men have only a single ulcer. Women frequently have four or more ulcers, with fewer symptoms.
The initial ulcer may be mistaken as a "hard" chancre, the typical sore of primary syphilis, as opposed to the "soft chancre" of chancroid.
Approximately one-third of the infected individuals will develop enlargements of the inguinal lymph nodes, the nodes located in the fold between the leg and the lower abdomen.
Half of those who develop swelling of the inguinal lymph nodes will progress to a point where the nodes rupture through the skin, producing draining abscesses. The swollen lymph nodes and abscesses are often referred to as buboes.
Sites
Males
- Internal and external surface of prepuce.
- Coronal sulcus
- Frenulum
- Shaft of penis
- Prepucial orifice
- Urethral meatus
- Glans penis
Females
- Labia majora is most common site. "Kissing ulcers" may develop. These are ulcers that occur on opposing surfaces of the labia.
- Labia minora
- Fourchette
- Vestibule
- Clitoris
- Perineal area
- Inner thighs
Diagnosis
Clinical variants
Some of clinical variants are as follows.[5]
| Variant | Characteristics |
|---|---|
| Dwarf chancroid | Small, superficial, relatively painless ulcer. |
| Giant chancroid | Large granulomatous ulcer at the site of a ruptured inguinal bubo, extending beyond its margins. |
| Follicular chancroid | Seen in females in association with hair follicles of the labia majora and pubis; initial follicular pustule evolves into a classic ulcer at the site. |
| Transient chancroid | Superficial ulcers that may heal rapidly,followed by a typical inguinal bubo. |
| Serpiginous chancroid | Multiple ulcers that coalesce to form a serpiginous pattern. |
| Mixed chancroid | Nonindurated tender ulcers of chancroid appearing together with an indurated nontender ulcer of syphilis having an incubation period of 10 to 90 days. |
| Phagedenic chancroid | Ulceration that causes extensive destruction of genitalia following secondary or superinfection by anaerobes such as Fusobacterium or Bacteroides. |
| Chancroidal ulcer | Most often a tender, nonindurated, single large ulcer caused by organisms other than Haemophilus ducreyi; lymphadenopathy is conspicuous by its absence. |
Laboratory findings
From bubo pus or ulcer secretions, H. ducreyi can be identified. PCR-based identification of organisms is available. Simple, rapid, sensitive and inexpensive antigen detection methods for H. ducreyi identification are also popular. Serologic detection of H. ducreyi is and uses outer membrane protein and lipooligosaccharide.
Differential diagnosis
- Patient has one or more painful genital ulcers. The combination of a painful ulcer with tender adenopathy is suggestive of chancroid; the presence of suppurative adenopathy is almost pathognomonic.
- No evidence of Treponema pallidum infection by darkfield microscopic examination of ulcer exudate or by a serologic test for syphilis performed greater than or equal to 7 days after onset of ulcers and
- Either a clinical presentation of the ulcer(s) not typical of disease caused by herpes simplex virus (HSV) or a culture negative for HSV.
Despite many distinguishing features, the clinical spectrums of following diseases may overlap with chancroid:
Comparison with syphilis
There are many differences and similarities between the conditions syphilitic chancre and chancroid.
- Similarities
- Both originate as pustules at the site of inoculation, and progress to ulcerated lesions
- Both lesions are typically 1–2 cm in diameter
- Both lesions are caused by sexually transmissible organisms
- Both lesions typically appear on the genitals of infected individuals
- Both lesions can be present at multiple sites and with multiple lesions
- Differences
- Chancre is a lesion typical of infection with the bacterium that causes syphilis, Treponema pallidum
- Chancroid is a lesion typical of infection with the bacterium Haemophilus ducreyi
- Chancres are typically painless, whereas chancroid are typically painful
- Chancres are typically non-exudative, whereas chancroid typically have a grey or yellow purulent exudate
- Chancres have a hard (indurated) edge, whereas chancroid have a soft edge
- Chancres heal spontaneously within three to six weeks, even in the absence of treatment
- Chancres can occur in the pharynx as well as on the genitals
Treatment
The CDC recommendation for chancroid is a single oral dose (1 gram) of azithromycin, or a single IM dose of ceftriaxone, or oral erythromycin for seven days.
Abscesses are drained.
H. ducreyi is resistant to sulfonamides, tetracyclines, penicillins, chloramphenicol, ciprofloxacin, ofloxacin, trimethoprim and aminoglycosides. Recently, several erythromycin resistant isolates have been reported.[5]
Treatment failure is possible with HIV co-infection and extended therapy is sometimes required.
Complications
- Extensive adenitis may develop.
- Large inguinal abscesses may develop and rupture to form draining sinus or giant ulcer.
- Superinfection by Fusarium and Bacteroides. These later require debridement and may result in disfiguring scars.
- Phimosis can develop in long standing lesion by scarring and thickening of foreskin, which may subsequently require circumcision.
Prevention
Chancroid spreads in populations with high sexual activity, such as prostitutes. Use of condom, prophylaxis by azithromycin, syndromic management of genital ulcers, treating patients with reactive syphilis serology are some of the strategies successfully tried in Thailand.[5]
Prognosis
Prognosis is excellent with proper treatment. Treating sexual contacts of affected individual helps break cycle of infection.
History
Chancroid has been known to humans since time of ancient Greeks.[7] Some of important events on historical timeline of chancre are:
| Year | Event |
|---|---|
| 1852 | Leon Bassereau distinguished chancroid from syphilis (i.e. soft chancre from hard chancre) |
| 1890s | Augusto Ducrey identified H. ducreyi |
| 1900 | Benzacon and colleagues isolated H. ducreyi |
| 1970s | Hammond and colleagues developed selective media |
External links
- Vaccine Shown Effective Against Chancroid in Medical News Today (May 9, 2006). Retrieved on May 1, 2008.
References
- ↑ James, William D.; Berger, Timothy G.; et al. (2006). Andrews' Diseases of the Skin: clinical Dermatology. Saunders Elsevier. p. 274. ISBN 0-7216-2921-0.
- ↑ Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 1-4160-2999-0.
- ↑ http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1446372/. Missing or empty
|title=(help); External link in|website=(help); - ↑ http://pathmicro.med.sc.edu/infectious%20disease/sexually%20transmitted%20diseases.htm
- 1 2 3 4 CURRENT Diagnosis & Treatment of Sexually Transmitted Diseases. McGraw-Hill Companies,Inc. 2007. pp. 69–74. ISBN 9780071509619.
- ↑ Medical Microbiology: The Big Picture. McGraw Hill Professional. p. 243. ISBN 9780071476614.
- ↑ Sexually Transmitted Diseases, 4th ed. McGraw Hill Professional. 2007. pp. 689–698. ISBN 9780071417488.
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||