Video-assisted thoracoscopic surgery
| Video-assisted thoracoscopic surgery | |
|---|---|
| Intervention | |
_CRUK_378.svg.png) Diagram showing video assisted thoracoscopy (VATS) | |
| MeSH | D020775 |
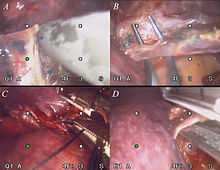
Video-assisted thoracoscopic surgery (VATS) is a type of thoracic surgery performed using a small video camera that is introduced into the patient's chest via a scope. The surgeon is able to view the instruments that are being used along with the anatomy on which the surgeon is operating. The camera and instruments are inserted through separate holes in the chest wall also known as "ports". These small ports are advantageous because the chance for infection and wound dehiscence are drastically reduced. This allows for a faster recovery by the patient and a greater chance for the wound to heal.[1]
Traditionally, thoracic surgery performed for diagnosis or treatment of chest conditions has required access to the chest through thoracotomy or sternotomy incisions. Sternotomy requires the use of a sternal saw to divide the sternum and requires spreading of the divided portions of the sternum with a sternal retractor to allow for visualization of the thoracic structures, passage of instruments into the chest, and removal of specimens. Thoracotomy, as most commonly performed, requires division of one or more major muscles of the chest wall including the latissimus dorsi, pectoralis or serratus muscles, along with spreading of the ribs with a rib spreader. Because the joints of the ribs with the vertebral bodies have only limited flexibility, the use of a rib spreader usually results in rib fractures in the process of rendering the interspace between the ribs wide enough to perform diagnostic or therapeutic maneuvers. Because of this, thoracic surgeons generally intentionally remove a section of one or more ribs in an effort to prevent splintered rib fractures associated with the use of a rib spreader. Sternotomy and thoracotomy have been proven over decades to provide highly effective means of access to thoracic structures and in general are tolerated by patients. However, both incisions have the potential for causing significant pain that may last for extended periods and both result in bony fractures that require a minimum of six weeks to heal during which time patients must refrain from heavy lifting or strenuous activity. The great advantage of VATS over sternotomy or thoracotomy is avoidance of muscle division and bone fractures that allows for diminished duration and intensity of pain and a shorter time to return to full activity.
VATS came into widespread use beginning in the early 1990s. Operations that traditionally were carried out with thoracotomy or sternotomy that today can be performed with VATS include: biopsy for diagnosis of pulmonary, pleural or mediastinal pathology; decortication for empyema; pleurodesis for recurrent pleural effusions or spontaneous pneumothorax; surgical stapler assisted wedge resection of lung masses; resection of mediastinal or pleural masses; thoracic sympathectomy for hyperhidrosis; operations for diaphragmatic hernias or paralysis; esophageal resection or resection of esophageal masses or diverticula; and VATS lobectomy/mediastinal lymphadenectomy for lung cancer.[1]
The instrumentation for VATS includes the use of a camera-linked 5mm or 10mm fiber-optic scope, with or without a 30 degree angle of visualization, and either conventional thoracic instruments or laparoscopic instruments. Unlike with laparoscopy, carbon dioxide insufflation is not generally required with VATS due to the inherent vault-like shape of the thoracic cavity. However, lung deflation on the side of the chest where VATS is being performed is a must to be able to visualize and pass instruments into the thorax; this is usually effected with a double-lumen endo-tracheal tube that allows for single lung ventilation or a bronchial blocker delivered via a standard single-lumen endotracheal tube.[1]
Similarly to laparoscopy, VATS has enjoyed widespread use for technically straightforward operations such as pulmonary decortication, pleurodesis, and lung or pleural biopsies, while more technically demanding operations such as esophageal operations, mediastinal mass resections, or pulmonary lobectomy for early stage lung cancer, have been slower to catch on and have tended to remain confined to selected centers. It is expected that advanced VATS techniques will continue to grow in numbers spurred by patient demand and greater surgeon comfort with the techniques.
See also
- Thoracic surgery
- VATS lobectomy
References
Further reading
- Calvin SH Ng, Song Wan, Tak Wai Lee, Innes YP Wan, Ahmed Arifi, Anthony PC Yim. Video-assisted thoracic surgery in spontaneous pneumothorax. Can Respir J 2002;9:122-127
- Calvin SH Ng, Song Wan, Tak Wai Lee, Alan DL Sihoe, Innes YP Wan, Ahmed A Arifi, Anthony PC Yim. Video assisted thoracoscopic surgery for mediastinal extramedullary haematopoiesis. Ann R Coll Surg Engl 2002;84:161-163
- Calvin SH Ng, Song Wan, Anthony PC Yim. Paradigm shift in surgical approaches to spontaneous pneumothorax: VATS. Thorax 2004;59:357
- Calvin SH Ng, Tak Wai Lee, Song Wan, Innes YP Wan, Alan DL Sihoe, Ahmed A Arifi, Anthony PC Yim. Thoracotomy is associated with significantly more profound suppression in Lymphocytes and Natural Killer cells than Video-Assisted Thoracic Surgery following major lung resections for cancer. J Invest Surg 2005;18:81-88
- Calvin SH Ng, Tak Wai Lee, Song Wan, Anthony PC Yim. Video-Assisted Thoracic Surgery in the Management of Spontaneous Pneumothorax: The Current Status. Postgrad Med J 2006;82:179-185
- Calvin SH Ng, Song Wan, Malcolm J Underwood, Anthony PC Yim. VATS and Extramedullary Haematopoiesis. Eur Resp J 2006;28:255-6
- Juan C Garzon, Calvin SH Ng, Alan D Sihoe, Anthony V Manlulu, Randolph HL Wong, Tak Wai Lee, Anthony PC Yim. Video-Assisted Thoracic Surgery Pulmonary Resection for Lung Cancer in Patients with Poor Lung Function. Ann Thorac Surg 2006;81:1996-2003
- Calvin SH Ng, Anthony PC Yim. Spontaneous Hemopneumothorax. Curr Opin Pulm Med 2006;12:273-277
- Calvin SH Ng, Song Wan, Connie WC Hui, Tak Wai Lee, Malcolm J Underwood, Anthony PC Yim. Video-Assisted Thoracic Surgery for Early Stage Lung Cancer – Can short-term immunological advantages improve long-term survival? Ann Thorac Cardiovasc Surg 2006;12:308-12
- Calvin SH Ng, Song Wan, Connie WC Hui, Innes YP Wan, Tak Wai Lee, Malcolm J Underwood, Anthony PC Yim. VATS lobectomy for lung cancer is associated with less immunochemokine disturbances than thoracotomy. Eur J Cardiothorac Surg 2007;31:83-7
- Juan C Garzon, Calvin SH Ng, Tak Wai Lee, Anthony PC Yim. Video-assisted Thoracic Surgery for Pneumothorax in LAM. Heart Lung Circ 2007;16: 300-302
- Calvin SH Ng, Innes YP Wan, Anthony PC Yim. Impact of Video-Assisted Thoracoscopic Major Lung Resection on Immune Function. Asian Cardiovasc Thorac Annals 2009;17:426-432
- Calvin SH Ng, Anthony PC Yim. Videothoracoscopic Approach to Posterior Mediastinal Tumors. Mineo TC (eds). Thoracic Surgery Clinics 2010 May; 20(2):297-309
- Calvin SH Ng, Innes YP Wan, Anthony PC Yim. VATS Thymectomy- The Better Approach. Ann Thorac Surg 2010;89: S2135
- Wong RHL, Ng CSH, Wong JKW, Tsang S. Needlescopic video-assisted thoracic surgery for reversal of thoracic sympathectomy. Interact CardioVasc Thorac Surg 2012;14:350-2
- Ng CSH, Wong RHL, Yeung ECL, Kwok MWT, Lau RWH, Ho AMH, Yim APC, Underwood MJ. Needlescopic Video-Assisted Thoracoscopic Pericardial Window. Surgical Practice 2012;16(2):84-5
- Ng CSH, Wan S, Wong RHL, Ho AMH, Yim APC. Angiogenic Response to Major Lung Resection for Non-Small Cell Lung Cancer with Video-Assisted Thoracic Surgical and Open Access. ScientificWorldJournal. 2012;2012:636754
- Ng CSH, Yeung ECL, Wong RHL, Kwok WT. Single-port Sympathectomy for Palmar Hyperhidrosis with VasoView: HemoPro 2 Endoscopic Vein Harvesting Device. J Thorac Cardiovasc Surg. 2012 Nov;144(5):1256-7
- Ng CSH, Hui JWY, Wong RHL. Minimizing Single Port Access in VATS Wedge Resection by Hookwire. Asian Cardiovasc Thorac Annals 2013;21(1):114-115
- Ng CSH, Lau KKW, Gonzalez-Rivas D, Rocco G. Evolution in Surgical Approach & Techniques for Lung Cancer. Thorax 2013;68:681
- Ng CSH. Uniportal VATS in Asia. J Thorac Dis 2013;5(S3):S221-S225
- Ng CSH, Lau RWH, Wong RHL, Yim APC. Evolving Techniques of Endoscopic Thoracic Sympathectomy: Smaller Incisions or Less? The Surgeon 2013;11:290-291
- Ng CSH, Lau RWH, Wong RHL, Ho AMH, Wan S. Single Port Vasoview Ò Sympathectomy for Palmar Hyperhidrosis: A Clinical Update. Journal of Laparoendoscopic & Advanced Surgical Techniques 2014;24(1):32-4
- Ng CSH, Wong RHL, Lau RWH, Yim APC. Minimizing Chest Wall Trauma in Single Port Video-Assisted Thoracic Surgery. J Thorac Cardiovasc Surg 2014;147(3):1095-6
| ||||||||||||||||||||||||