Health care in New Zealand
The healthcare system of New Zealand has undergone significant changes throughout the past several decades. From an essentially fully public system in the early 20th century, reforms have introduced market and health insurance elements primarily in the last three decades, creating a mixed public-private system for delivering healthcare.
- The Accident Compensation Corporation covers the costs of treatment for cases deemed 'accidents', including medical misadventure, for all people legally in New Zealand (including tourists). The costs are recovered via levies on employers, employees, petrol and vehicle registration, and contributions from the general tax pool.
- The relatively extensive and high-quality system of public hospitals treats citizens or permanent residents free of charge and is managed by District Health Boards. However, costly or difficult operations often require long waiting list delays unless the treatment is medically urgent.[1] Because of this, a secondary market of health insurance schemes exists which fund operations and treatments for their members privately. Southern Cross Health Insurance, a non-profit-scheme, is the largest of these at about 60% of the health insurance market and covering almost a quarter of all New Zealanders in 2007, even operating its own chain of hospitals.[2]
- Primary care (non-specialist doctors / family doctors) and medications on the list of the New Zealand government agency PHARMAC require co-payments, but are subsidised, especially for patients with community health services cards or high user health cards.
- Emergency services are primarily provided by St. John New Zealand charity (as well as Wellington Free Ambulance in the Wellington Region), supported with a mix of private (donated) and public (subsidy) funds.
In 2012, New Zealand spent 8.7% of GDP on health care, or US$3,929 per capita. Of that, approximately 77% was government expenditure.[3] In a 2010 study, New Zealand came last in a study for the level of medications use in 14 developed countries (i.e. used least medicines overall), and also spent the lowest amount on healthcare amongst the same list of countries, with US$2510 ($3460) per capita, compared to the United States at US$7290.[4]
Structure
The Ministry of Health is responsible for the oversight and funding of the twenty District Health Boards (DHBs). These are responsible for organizing healthcare in the district and meeting the standards set by the Ministry of Health. Twenty-one DHBs came into being on January 1, 2001 with Southland and Otago DHBs merging into Southern DHB on 1 May 2010.
The boards for each DHB are elected in elections held every three years, with the exception of one of the eight board members, who is appointed by the Ministry of Health.
The DHBs oversee the forty six Primary Health Organizations established throughout the country. These were first set up in July, 2002, with a mandate to focus on the health of communities. Originally there were 81 of these, but this has been reduced down to 46 in 2008. They are funded by DHBs, and are required to be entirely non-profit, democratic bodies that are responsive to their communities' needs. Almost all New Zealanders are enrolled in a PHO, as there are financial incentives for the patients to become enrolled.
The Northern Region DHBs also use shared seervices provided by the Northern DHB Support Agency and HealthAlliance. These services deliver region wide health initiatives and shared IT services and logistics.
Public vs. private payment
The burden for the core of the healthcare system rests with government expenditure (approx. 77%).[3] Private payment by individuals also plays an important role in the overall system although the cost of these payments are comparatively minor.
Damage as a result of "accidents", ranging from minor to major physical and psychological trauma, is generally completely covered by the Accident Compensation Corporation (ACC). This may include coverage for doctors visits and lump-sum payments.
Those earning less than certain amounts, depending on the number of dependents in their household, can qualify for a Community Services Card (CSC), which reduces the upfront fee for visiting a doctor.
Hospital and specialist care, on the other hand, is totally covered by the government if the patient is referred by a general or family practitioner.
Health statistics
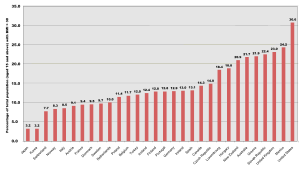
The following statistics are a sample from the World Health Organization Statistical Information System (WHOSIS). The year on which the data were sampled follows the statistic in brackets.
- Demographics
- Population (in thousands): 4,460 (2012)
- Total fertility rate (per woman): 2.07 (2012)
- Adolescent fertility rate (%): 27 (2004)
- Funding
- Per capita government spending (PPP Int $): 1,905 (2006)
- Per capita total spending (PPP Int $): 2,447 (2006)
- Total expenditure (% of GDP): 9.4 (2006)
- Life expectancy
- Life expectancy at birth (years): 82 (2012)
- Life expectancy for females (years): 84 (2012)
- Life expectancy for males (years): 80 (2012)
- Neonatal mortality (per 1,000 live births): 3 (2012)
- Infant mortality (per 1,000 live births): 5 (2012)
- Years of life lost to communicable diseases (%): 5 (2002)
- Years of life lost to injuries (%): 17 (2002)
- Years of life lost to non-communicable diseases (%): 79 (2002)
Abortion
Abortion is legal in New Zealand, if certain criteria are met. In general, either the health of the mother or the foetus must be in jeopardy. Additionally, two doctors must give their consent to the procedure. There were 18,380 abortions carried out in 2007, following a general increase in both the absolute number and per capita rate since 1991.
Medications
The Pharmaceutical Management Agency of New Zealand (PHARMAC) was set up in 1993 to decide which medications the government will subsidise. In general, PHARMAC will select an effective and safe medication from a class of drugs, and negotiate with the drug manufacturer to obtain the best price. There are approximately 2,000 drugs listed on the national schedule that are either fully or partially subsidised.
Emergency service
Outside the Wellington Region, Emergency and non-urgent ambulance transportation is carried out by the charitable organization St. John New Zealand. In Greater Wellington Region ambulance services are provided by the Wellington Free Ambulance organisation.
See also
- Euthanasia in New Zealand
- HIV/AIDS in New Zealand
- Water safety in New Zealand
- List of New Zealand doctors
References
- ↑ "OECD iLibrary: Statistics / Health at a Glance / 2011 / Waiting time of four months or more for elective surgery". Organisation for Economic Cooperation and Development (OECD). Retrieved 2012-12-27.
- ↑ Hudson, Alice (14 October 2007). "Health cover under the knife". The New Zealand Herald. Retrieved 2 October 2011.
- ↑ 3.0 3.1 "WHO Statistical Information System". World Health Organization. Retrieved 2008-09-23.
- ↑ Johnston, Martin (30 July 2010). "NZ ranks last in medicine use and lowest health spender". The New Zealand Herald. Retrieved 30 July 2010.
Further reading
- Gerritsen, Sarah; Niki Stefanogiannis; Yvonne Galloway (2008). A portrait of health key results of the 2006/07 New Zealand health survey. Wellington, N.Z.: Ministry of Health. ISBN 978-0-478-31741-1. Retrieved 2012-01-21.
External links
- New Zealand Ministry of Health
- World Health Organization Statistical Information System (WHOSIS)
- Pharmaceutical Management Agency of New Zealand (PHARMAC)
| ||||||||||||||