Hypercholesterolemia
| Hypercholesterolemia | |
|---|---|
| Classification and external resources | |
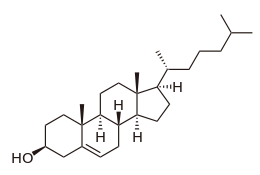 Formula structure of cholesterol | |
| ICD-10 | E78.0 |
| ICD-9 | 272.0 |
| DiseasesDB | 6226 |
| MedlinePlus | 000403 |
| eMedicine | med/1073 |
| MeSH | D006937 |
Hypercholesterolemia (also spelled hypercholesterolaemia) is the presence of high levels of cholesterol in the blood.[1] It is a form of "hyperlipidemia" (elevated levels of lipids in the blood) and "hyperlipoproteinemia" (elevated levels of lipoproteins in the blood).[1]
Cholesterol is a sterol; see the diagrammatic structure at the right. It is one of three major classes of lipids which all animal cells utilize to construct their membranes and is thus manufactured by all animal cells. Plant cells do not manufacture cholesterol. It is also the precursor of the steroid hormones, bile acids and vitamin D.
Since cholesterol is insoluble in water, it is transported in the blood plasma within protein particles (lipoproteins). Lipoproteins are classified by their density: very low density lipoprotein (VLDL), intermediate density lipoprotein (IDL), low density lipoprotein (LDL) and high density lipoprotein (HDL).[2] All the lipoproteins carry cholesterol, but elevated levels of the lipoproteins other than HDL (termed non-HDL cholesterol), particularly LDL-cholesterol are associated with an increased risk of atherosclerosis and coronary heart disease.[3] In contrast higher levels of HDL cholesterol are protective.[4] Elevated levels of non-HDL cholesterol and LDL in the blood may be a consequence of diet, obesity, inherited (genetic) diseases (such as LDL receptor mutations in familial hypercholesterolemia), or the presence of other diseases such as diabetes and an underactive thyroid.[1]
Reducing dietary fat is recommended to reduce total blood cholesterol and LDL in adults.[5] In people with very high cholesterol (e.g. familial hypercholesterolemia), diet is often insufficient to achieve the desired lowering of LDL and lipid lowering medications which reduce cholesterol production or absorption are usually required.[6] If necessary, other treatments such as LDL apheresis or even surgery (for particularly severe subtypes of familial hypercholesterolemia) are performed.[6]
Signs and symptoms

Although hypercholesterolemia itself is asymptomatic, longstanding elevation of serum cholesterol can lead to atherosclerosis.[7] Over a period of decades, chronically elevated serum cholesterol contributes to formation of atheromatous plaques in the arteries. This can lead to progressive stenosis (narrowing) or even complete occlusion (blockage) of the involved arteries. Alternatively smaller plaques may rupture and cause a clot to form and obstruct blood flow.[8] A sudden occlusion of a coronary artery results in a myocardial infarction or heart attack. An occlusion of an artery supplying the brain can cause a stroke. If the development of the stenosis or occlusion is gradual blood supply to the tissues and organs slowly diminishes until organ function becomes impaired. At this point that tissue ischemia (restriction in blood supply) may manifest as specific symptoms. For example, temporary ischemia of the brain (commonly referred to as a transient ischemic attack) may manifest as temporary loss of vision, dizziness and impairment of balance, aphasia (difficulty speaking), paresis (weakness) and paresthesia (numbness or tingling), usually on one side of the body. Insufficient blood supply to the heart may manifest as chest pain, and ischemia of the eye may manifest as transient visual loss in one eye. Insufficient blood supply to the legs may manifest as calf pain when walking, while in the intestines it may present as abdominal pain after eating a meal.[1][9]
Some types of hypercholesterolemia lead to specific physical findings. For example, familial hypercholesterolemia (Type IIa hyperlipoproteinemia) may be associated with xanthelasma palpebrarum (yellowish patches underneath the skin around the eyelids),[10] arcus senilis (white or gray discoloration of the peripheral cornea),[11] and xanthomata (deposition of yellowish cholesterol-rich material) of the tendons, especially of the fingers.[12][13] Type III hyperlipidemia may be associated with xanthomata of the palms, knees and elbows.[12]
Causes
Hypercholesterolemia is typically due to a combination of environmental and genetic factors.[7] Environmental factors include obesity and dietary choices.[7] Genetic contributions are usually due to the additive effects of multiple genes, though occasionally may be due to a single gene defect such as in the case of familial hypercholesterolaemia.[7] A number of secondary causes exist including: diabetes mellitus type 2, obesity, alcohol, monoclonal gammopathy, dialysis, nephrotic syndrome, obstructive jaundice, hypothyroidism, Cushing’s syndrome, anorexia nervosa, medications (thiazide diuretics, ciclosporin, glucocorticoids, beta blockers, retinoic acid).[7]
Diet

Diet has an important effect on blood cholesterol but the size of this effect varies substantially between individuals.[14] Approximately 50% of non-esterified cholesterol is absorbed in the intestine,[15] but inter-individual variations in the efficiency of uptake, and the effect of other dietary components such as plant sterols and fiber content affect absorption.[15] Moreover, when dietary cholesterol intake goes down, production (principally by the liver[16]) typically increases, though not always with complete compensation, so that reductions in blood cholesterol can be modest. Reductions in fat intake, particularly saturated fats, also reduce blood cholesterol.[17] Dietary sucrose and fructose can raise LDL cholesterol levels in the blood.[18] In the United States, the National Lipid Association Expert Panel on Familial Hypercholesterolemia recommends that people with familial hypercholesterolemia restrict intakes of total fat to 25 - 35% of energy intake; that saturated fatty acids should make up less than 7% of energy intake, and that cholesterol intake should be less than 200 mg per day.[6] There is also evidence that inclusion of 2 g per day of plant stanol or sterol esters and 10 to 20 g per day of soluble fiber decrease dietary cholesterol absorption.[6] Dietary changes can typically achieve reductions of 10 to 15% in blood cholesterol.[6]
Maintaining a healthy body weight through increased physical activity and appropriate caloric intake is also important. Overweight or obese individuals can lower blood cholesterol by losing weight - on average a kilogram of weight loss can reduce LDL cholesterol by 0.8 mg/dL.[6]
Genetics
Genetic abnormalities are in some cases completely responsible for hypercholesterolemia, such as in familial hypercholesterolemia where there is one or more genetic mutations in the autosomal dominant APOB gene, the autosomal recessive LDLRAP1 gene, autosomal dominant familial hypercholesterolemia (HCHOLA3) variant of the PCSK9 gene, or the LDL receptor gene.[19]
Even when there is no single mutation responsible for hypercholesterolemia, genetic predisposition still plays a major role in combination with sedentary lifestyle, obesity, or an atherogenic diet.[20]
Diagnosis
| Interpretation of Cholesterol levels | |||
|---|---|---|---|
| cholesterol type | mg/dL | mmol/L | interpretation |
| total cholesterol | under 200 | under 5.2 | desirable[21] |
| 200-239 | 5.2-6.2 | borderline[21] | |
| over 240 | over 6.2 | high[21] | |
| LDL cholesterol | under 100 | under 2.6 | most desirable[21] |
| 100-129 | 2.6-3.3 | good[21] | |
| 130-159 | 3.4-4.1 | borderline high[21] | |
| 160-189 | 4.1-4.9 | high and undesirable[21] | |
| over 190 | over 4.9 | very high[21] | |
| HDL cholesterol | under 40 | under 1.0 | undesirable; risk increased[21] |
| 41-59 | 1.0-1.5 | okay, but not optimal[21] | |
| over 60 | over 1.55 | good; risk lowered[21] | |
| Indications to lower LDL cholesterol | |||
|---|---|---|---|
| Persons whose coronary risk is... | because they have... | should consider lowering LDL if the level is over... | and LDL reduction is indicated if the level is over... |
| high | greater than 20% risk of heart attack in 10 years, or an extreme risk factor such as coronary heart disease, diabetes, peripheral-artery disease, carotid-artery disease, or aortic aneurysm | 70 mg/dL, 3.88 mmol/dL especially if there are risk factors[22] | 100 mg/dL, 5.55 mmol/dL[22] |
| moderately high | a 10-20% risk of heart attack in 10 years and two or more risk factors | 100 mg/dL, 5.55 mmol/dL[22] | 130 mg/dL, 7.21 mmol/dL[22] |
| moderate | less than 10% risk of heart attack in 10 years and two or more risk factors | 130 mg/dL, 7.21 mmol/dL[22] | 160 mg/dL, 8.88 mmol/dL[22] |
| low | No risk factors or only one | 160 mg/dL, 8.88 mmol/dL[22] | 190 mg/dL, 10.5 mmol/dL[22] |
Cholesterol is measured as milligrams per deciliter (mg/dL) of blood in the United States and some other countries. In the United Kingdom, most European countries, and Canada, millimoles per liter of blood (mmol/L) is the measure.[23]
For healthy adults, the UK National Health Service recommends total cholesterol of 5 mmol/L or less, and low-density lipoprotein cholesterol (LDL) of 3 mmol/L or less. For people at high risk of cardiovascular disease, the recommendation for total cholesterol is 4 mmol/L or less, and 2 mmol/L or less for LDL.[24]
In the United States, the National Heart, Lung, and Blood Institute within the National Institutes of Health classifies total cholesterol of less than 200 mg/dL as “desirable,” 200 to 239 mg/dL as “borderline high,” and 240 mg/dL or more as “high.”[25]
There is not an absolute cutoff between normal and abnormal cholesterol levels and interpretation of values needs to be made in relation to other health conditions and risk factors.
Higher levels of total cholesterol increase the risk of cardiovascular disease, particularly coronary heart disease. Levels of LDL or non-HDL cholesterol both predict future coronary heart disease, which is the better predictor is disputed.[26] High levels of small dense LDL may be particularly adverse, although measurement of small dense LDL is not advocated for risk prediction.[26] In the past LDL and VLDL levels were rarely measured directly due to cost. Levels of fasting triglycerides were taken as an indicator of VLDL levels (generally about 45% of fasting triglycerides is composed of VLDL), while LDL was usually estimated by the Friedewald formula:
LDL  total cholesterol - HDL - (0.2 x fasting triglycerides).
total cholesterol - HDL - (0.2 x fasting triglycerides).
However, this equation is not valid on non-fasting blood samples or if fasting triglycerides are elevated >4.5 mmol/L (> ∼400 mg/dL). Recent guidelines have therefore advocated the use of direct methods for measurement of LDL wherever possible.[26] It may be useful to measure all lipoprotein subfractions ( VLDL, IDL, LDL, HDL) when assessing hypercholesterolemia and measurement of apolipoproteins and lipoprotein (a) can also be of value.[26] Genetic screening is now advised if a form of familial hypercholesterolemia is suspected.[26]
Classification
Classically, hypercholesterolemia was categorized by lipoprotein electrophoresis and the Fredrickson classification. Newer methods, such as "lipoprotein subclass analysis" have offered significant improvements in understanding the connection with atherosclerosis progression and clinical consequences.
If the hypercholesterolemia is hereditary (familial hypercholesterolemia), there is more often a family history of premature, earlier onset atherosclerosis.
Screening
The U.S. Preventive Services Task Force (USPSTF) strongly recommends routine screening for men 35 years and older and women 45 years and older for lipid disorders and the treatment of abnormal lipids in people who are at increased risk of coronary heart disease. They also recommend routinely screening men aged 20 to 35 years and women aged 20 to 45 years if they have other risk factors for coronary heart disease.[27] In Canada screening is recommended for men 40 and older and women 50 and older.[28] In those with normal cholesterol levels screening is recommended once every five years.[29] Once people are on a statin further testing provides little benefit except to possibly determine compliance with treatment.[30]
Treatment
Recommendations for both primary prevention[31] and secondary prevention[32] have been published. For those at high risk a combination of lifestyle modification and statins has been shown to decrease mortality.[7]
Lifestyle
Lifestyle changes recommended for those with high cholesterol include: smoking cessation, limiting alcohol consumption, increasing physical activity, and maintaining a healthy weight. A diet that emphasizes low-cholesterol foods, restricts saturated fats,[7] and avoids trans fat is also recommended.[33] In strictly controlled surroundings, dietary changes can reduce cholesterol levels by 15 percent. In practice, dietary advice can provide a modest decrease in cholesterol levels and may be sufficient in the treatment of mildly elevated cholesterol.[34]
Medication
Statins (or HMG-CoA reductase inhibitors) are commonly used to treat hypercholesterolemia if diet is ineffective. Other agents that may be used include: fibrates, nicotinic acid and cholestyramine.[35] These however are only recommended if statins are not tolerated.[35] Statins can reduce total cholesterol by approximately 50% in the majority of people;[26] effects appear similar regardless of the statin used.[36] While statins are effective in decreasing mortality in those who have had previous cardiovascular disease, there is debate over whether or not they are effective in those with high cholesterol but no other health problems.[37] One review did not find a mortality benefit in those at high-risk but without prior cardiovascular disease.[37] Other reviews concluded that there is a mortality benefit[36][38][39] but concerns regarding the quality of the evidence persist.[40] With respect to quality of life there is limited evidence of improvement when statins are used in people without existing cardiovascular disease (i.e. for primary prevention).[40] Statins decrease cholesterol in children with hypercholesterolemia but no studies as of 2010 show improved clinical outcomes[41] and diet is the mainstay of therapy in childhood.[26]
Guidelines
Various clinical practice guidelines have addressed the treatment of hypercholesterolemia. The American College of Physicians has addressed hypercholesterolemia in patients with diabetes.[42] Their four recommendations are:
- Lipid-lowering therapy should be used for secondary prevention of cardiovascular mortality and morbidity for all patients (both men and women) with known coronary artery disease and type 2 diabetes.
- Statins should be used for primary prevention against macrovascular complications in patients (both men and women) with type 2 diabetes and other cardiovascular risk factors.
- Once lipid-lowering therapy is initiated, patients with type 2 diabetes mellitus should be taking at least moderate doses of a statin (the accompanying evidence report states "simvastatin, 40 mg/d; pravastatin, 40 mg/d; lovastatin, 40 mg/d; atorvastatin, 20 mg/d; or an equivalent dose of another statin").[43]
- For those patients with type 2 diabetes who are taking statins, routine monitoring of liver function tests or muscle enzymes is not recommended except in specific circumstances.
The National Cholesterol Education Program revised their guidelines;[44] however, their 2004 revisions have been criticized for use of nonrandomized, observational data.[45]
In the UK, the National Institute for Health and Clinical Excellence (NICE) has made recommendations for the treatment of elevated cholesterol levels, published in 2008.[35]
The Task Force for the management of dyslipidaemias of the European Society of Cardiology (ESC) and the European Atherosclerosis Society (EAS) published the ESC/EAS Guidelines for the management of dyslipidaemias in 2011.[26]
Alternative medicine
According to a survey in 2002, alternative medicine was used in an attempt to treat cholesterol by 1.1% of U.S. adults. Consistent with previous surveys, this one found that the majority of individuals (i.e., 55%) used it in conjunction with conventional medicine.[46] A review of trials of phytosterols and/or phytostanols reported an average of 9% lowering of LDL-cholesterol.[47] In 2000 the Food and Drug Administration approved the labeling of foods containing specified amounts of phytosterol esters or phytostanol esters as cholesterol lowering; in 2003 an FDA Interim Health Claim Rule extended that label claim to foods or dietary supplements delivering more than 0.8 grams/day of phytosterols or phytostanols. Some researchers, however, are concerned about diet supplementation with plant sterol esters and draw attention to lack of long-term safety data.[48]
Epidemiology
Rates of high total cholesterol in the United States in 2010 are just over 13% down from 17% in 2000.[49]
Average total cholesterol in the United Kingdom is 5.9 mmol/L while in rural China and Japan average total cholesterol is 4 mmol/L.[7] Rates of coronary artery disease are high in Great Britain, but low in rural China and Japan.[7]
References
- ↑ 1.0 1.1 1.2 1.3 Durrington, P (August 2003). "Dyslipidaemia". The Lancet 362 (9385): 717–31. doi:10.1016/S0140-6736(03)14234-1. PMID 12957096.
- ↑ Biggerstaff KD, Wooten JS (December 2004). "Understanding lipoproteins as transporters of cholesterol and other lipids". Adv Physiol Educ 28 (1–4): 105–6. doi:10.1152/advan.00048.2003. PMID 15319192.
- ↑ Carmena R, Duriez P, Fruchart JC (June 2004). "Atherogenic lipoprotein particles in atherosclerosis". Circulation 109 (23 Suppl 1): III2–7. doi:10.1161/01.CIR.0000131511.50734.44. PMID 15198959.
- ↑ Kontush A, Chapman MJ (March 2006). "Antiatherogenic small, dense HDL--guardian angel of the arterial wall?". Nat Clin Pract Cardiovasc Med 3 (3): 144–53. doi:10.1038/ncpcardio0500. PMID 16505860.
- ↑ Hooper L, Summerbell CD, Thompson R, et al. (2012). "Reduced or modified dietary fat for preventing cardiovascular disease". In Hooper, Lee. Cochrane Database Syst Rev 5: CD002137. doi:10.1002/14651858.CD002137.pub3. PMID 22592684.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 Ito MK, McGowan MP, Moriarty PM (June 2011). "Management of familial hypercholesterolemias in adult patients: recommendations from the National Lipid Association Expert Panel on Familial Hypercholesterolemia". J Clin Lipidol 5 (3 Suppl): S38–45. doi:10.1016/j.jacl.2011.04.001. PMID 21600528.
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 7.7 7.8 Bhatnagar D, Soran H, Durrington PN (2008). "Hypercholesterolaemia and its management". BMJ 337: a993. doi:10.1136/bmj.a993. PMID 18719012.
- ↑ Finn AV, Nakano M, Narula J, Kolodgie FD, Virmani R (July 2010). "Concept of vulnerable/unstable plaque". Arterioscler. Thromb. Vasc. Biol. 30 (7): 1282–92. doi:10.1161/ATVBAHA.108.179739. PMID 20554950.
- ↑ Grundy, SM; Balady, GJ; Criqui, MH; Fletcher, G; Greenland, P; Hiratzka, LF; Houston-Miller, N; Kris-Etherton, P; Krumholz, HM; Larosa, J.; Ockene, I. S.; Pearson, T. A.; Reed, J.; Washington, R.; Smith, S. C. (1998). "Primary prevention of coronary heart disease: guidance from Framingham: a statement for healthcare professionals from the AHA Task Force on Risk Reduction. American Heart Association". Circulation 97 (18): 1876–87. doi:10.1161/01.CIR.97.18.1876. PMID 9603549.
- ↑ Shields, C; Shields, J (2008). Eyelid, conjunctival, and orbital tumors: atlas and textbook. Hagerstown, Maryland: Lippincott Williams & Wilkins. ISBN 0-7817-7578-7.
- ↑ Zech LA Jr, Hoeg JM (2008-03-10). "Correlating corneal arcus with atherosclerosis in familial hypercholesterolemia". Lipids Health Dis 7: 7. doi:10.1186/1476-511X-7-7. PMC 2279133. PMID 18331643.
- ↑ 12.0 12.1 James, WD; Berger, TG (2006). Andrews' Diseases of the Skin: Clinical Dermatology. Saunders Elsevier. pp. 530–2. ISBN 0-7216-2921-0.
- ↑ Rapini, RP; Bolognia, JL; Jorizzo, JL (2007). Dermatology: 2-Volume Set. St. Louis, Missouri: Mosby. pp. 1415–6. ISBN 1-4160-2999-0.
- ↑ Howell WH, McNamara DJ, Tosca MA, Smith BT, Gaines JA (June 1997). "Plasma lipid and lipoprotein responses to dietary fat and cholesterol: a meta-analysis". Am. J. Clin. Nutr. 65 (6): 1747–64. PMID 9174470.
- ↑ 15.0 15.1 Lichtenstein AH (February 1990). "Intestinal cholesterol metabolism". Ann. Med. 22 (1): 49–52. doi:10.3109/07853899009147241. PMID 2184845.
- ↑ Stryer, Lubert; Berg, Jeremy Mark; Tymoczko, John L. (2007). Biochemistry. San Francisco: W.H. Freeman. ISBN 0-7167-8724-5.
- ↑ Sacks FM, Katan M (December 2002). "Randomized clinical trials on the effects of dietary fat and carbohydrate on plasma lipoproteins and cardiovascular disease". Am. J. Med. 113 Suppl 9B: 13S–24S. PMID 12566134.
- ↑ Schaefer, EJ; Gleason, JA; Dansinger, ML (June 2009). "Dietary fructose and glucose differentially affect lipid and glucose homeostasis". The Journal of nutrition 139 (6): 1257S–1262S. doi:10.3945/jn.108.098186. PMC 2682989. PMID 19403705.
- ↑ "Hypercholesterolemia". Genetics Home Reference. U.S. National Institutes of Health. Retrieved 5 December 2013.
- ↑ Citkowitz E, Isley WL (2010). "Polygenic Hypercholesterolemia". eMedicine. Medscape. Retrieved 2010-11-04.
- ↑ 21.0 21.1 21.2 21.3 21.4 21.5 21.6 21.7 21.8 21.9 21.10 Consumer Reports; Drug Effectiveness Review Project (March 2013). "Evaluating statin drugs to treat High Cholesterol and Heart Disease: Comparing Effectiveness, Safety, and Price". Best Buy Drugs (Consumer Reports): 9. Retrieved 27 March 2013, which cites
- United States Department of Health and Human Services; National Heart, Lung, and Blood Institute; National Institutes of Health (June 2005). "NHLBI, High Blood Cholesterol: What You Need to Know". nhlbi.nih.gov. Retrieved 27 March 2013.
- ↑ 22.0 22.1 22.2 22.3 22.4 22.5 22.6 22.7 Consumer Reports; Drug Effectiveness Review Project (March 2013). "Evaluating statin drugs to treat High Cholesterol and Heart Disease: Comparing Effectiveness, Safety, and Price". Best Buy Drugs (Consumer Reports): 9. Retrieved 27 March 2013, which cites
- Grundy, S. M.; Cleeman, J. I.; Merz, C. N.; Brewer Jr, H. B.; Clark, L. T.; Hunninghake, D. B.; Pasternak, R. C.; Smith Jr, S. C.; Stone, N. J.; for the Coordinating Committee of the National Cholesterol Education Program; Endorsed by the National Heart, Lung, and Blood Institute, American College of Cardiology Foundation, and American Heart Association (2004). "Implications of Recent Clinical Trials for the National Cholesterol Education Program Adult Treatment Panel III Guidelines". Circulation 110 (2): 227–239. doi:10.1161/01.CIR.0000133317.49796.0E. PMID 15249516.
- ↑ High Cholesterol – Tests and Diagnosis, Mayo Clinic staff. Retrieved 2013-03-09.
- ↑ Diagnosing High Cholesterol, NHS Choices. Retrieved 2013-03-09.
- ↑ ATP III Guidelines At-A-Glance Quick Desk Reference, National Cholesterol Education Program. Retrieved 2013-03-09.
- ↑ 26.0 26.1 26.2 26.3 26.4 26.5 26.6 26.7 Reiner Z, Catapano AL, De Backer G, et al. (July 2011). "ESC/EAS Guidelines for the management of dyslipidaemias: the Task Force for the management of dyslipidaemias of the European Society of Cardiology (ESC) and the European Atherosclerosis Society (EAS)". Eur. Heart J. 32 (14): 1769–818. doi:10.1093/eurheartj/ehr158. PMID 21712404.
- ↑ U.S. Preventive Services Task Force. "Screening for Lipid Disorders: Recommendations and Rationale". Retrieved 2010-11-04.
- ↑ Genest, J; Frohlich, J, Fodor, G, McPherson, R, Working Group on Hypercholesterolemia and Other, Dyslipidemias (2003-10-28). "Recommendations for the management of dyslipidemia and the prevention of cardiovascular disease: summary of the 2003 update". Canadian Medical Association Journal 169 (9): 921–4. PMC 219626. PMID 14581310.
- ↑ National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel, III) (2002-12-17). "Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) final report". Circulation 106 (25): 3143–421. PMID 12485966.
- ↑ Spector, R; Snapinn, SM (2011). "Statins for secondary prevention of cardiovascular disease: the right dose". Pharmacology 87 (1–2): 63–9. doi:10.1159/000322999. PMID 21228612.
- ↑ Pignone, M (2005). "Primary prevention: dyslipidaemia". Clin Evid (14): 142–50. PMID 16620402. Retrieved 2010-11-04.
- ↑ Gami, A (2006). "Secondary prevention of ischaemic cardiac events". Clin Evid (15): 195–228. PMID 16973010. Retrieved 2010-11-04.
- ↑ "How Can I Lower High Cholesterol". American Heart Association. Retrieved 2011-04-03.
- ↑ Tang JL, Armitage JM, Lancaster T, Silagy CA, Fowler GH, Neil HA (1998). "Systematic review of dietary intervention trials to lower blood total cholesterol in free-living subjects". BMJ 316 (7139): 1213–20. doi:10.1136/bmj.316.7139.1213. PMC 28525. PMID 9552999. Retrieved 2010-11-04.
- ↑ 35.0 35.1 35.2 National Institute for Health and Clinical Excellence. Clinical guideline 67: Lipid modification. London, 2008.
- ↑ 36.0 36.1 Tonelli, M; Lloyd, A, Clement, F, Conly, J, Husereau, D, Hemmelgarn, B, Klarenbach, S, McAlister, FA, Wiebe, N, Manns, B, for the Alberta Kidney Disease, Network (2011-11-08). "Efficacy of statins for primary prevention in people at low cardiovascular risk: a meta-analysis". CMAJ : Canadian Medical Association 183 (16): E1189–E1202. doi:10.1503/cmaj.101280. PMC 3216447. PMID 21989464.
- ↑ 37.0 37.1 Ray et al; Seshasai, S. R. K.; Erqou, S.; Sever, P.; Jukema, J. W.; Ford, I.; Sattar, N. (2010). "Statins and All-Cause Mortality in High-Risk Primary Prevention: A Meta-analysis of 11 Randomized Controlled Trials Involving 65 229 Participants". Arch Intern Med 170 (12): 1024–31. doi:10.1001/archinternmed.2010.182. PMID 20585067. Retrieved 2010-11-04.
- ↑ Mills, EJ; Wu, P, Chong, G, Ghement, I, Singh, S, Akl, EA, Eyawo, O, Guyatt, G, Berwanger, O, Briel, M (February 2011). "Efficacy and safety of statin treatment for cardiovascular disease: a network meta-analysis of 170,255 patients from 76 randomized trials". QJM : monthly journal of the Association of Physicians 104 (2): 109–24. doi:10.1093/qjmed/hcq165. PMID 20934984.
- ↑ Cholesterol Treatment Trialists' (CTT) Collaborators (2012). "The effects of lowering LDL cholesterol with statin therapy in people at low risk of vascular disease: meta-analysis of individual data from 27 randomised trials". Lancet. Online first. doi:10.1016/S0140-6736(12)60367-5.
- ↑ 40.0 40.1 Taylor F, Ward K, Moore TH, et al. (2011). "Statins for the primary prevention of cardiovascular disease". In Taylor, Fiona. Cochrane Database Syst Rev (1): CD004816. doi:10.1002/14651858.CD004816.pub4. PMID 21249663.
- ↑ Lebenthal Y, Horvath A, Dziechciarz P, Szajewska H, Shamir R (2010). "Are treatment targets for hypercholesterolemia evidence based? Systematic review and meta-analysis of randomised controlled trials". Arch Dis Child 95 (9): 673–80. doi:10.1136/adc.2008.157024. PMID 20515970.
- ↑ Snow V, Aronson M, Hornbake E, Mottur-Pilson C, Weiss K (2004). "Lipid control in the management of type 2 diabetes mellitus: a clinical practice guideline from the American College of Physicians". Ann Intern Med 140 (8): 644–9. doi:10.1059/0003-4819-140-8-200404200-00012. PMID 15096336. Retrieved 2010-11-04.
- ↑ Vijan, S; Hayward, RA; American College Of, Physicians (2004). "Pharmacologic lipid-lowering therapy in type 2 diabetes mellitus: background paper for the American College of Physicians". Ann Intern Med 140 (8): 650–8. doi:10.1059/0003-4819-140-8-200404200-00013. PMID 15096337. Retrieved 2010-11-04.
- ↑ Grundy SM, Cleeman JI, Merz CN, Brewer HB, Clark LT, Hunninghake DB, Pasternak RC, Smith SC, Stone NJ (2004). "Implications of recent clinical trials for the National Cholesterol Education Program Adult Treatment Panel III Guidelines". J Am Coll Cardiol 44 (3): 720–32. doi:10.1016/j.jacc.2004.07.001. PMID 15358046.
- ↑ Hayward, RA; Hofer, TP; Vijan, S (2006). "Narrative review: lack of evidence for recommended low-density lipoprotein treatment targets: a solvable problem". Ann Intern Med 145 (7): 520–30. doi:10.7326/0003-4819-145-7-200610030-00010. PMID 17015870.
- ↑ Barnes PM, Powell-Griner E, McFann K, Nahin RL (May 27, 2004). "Complementary and Alternative Medicine Use Among Adults: United States, 2002" (PDF). Advance Data from Vital and Health Statistics. http://nccam.nih.gov/news/2004/052704.htm (343): 6–9. Retrieved 2010-11-04.
- ↑ Demonty I, Ras RT, van der Knaap HC, Duchateau GS, Meijer L, Zock PL, Geleijnse JM, Trautwein EA (February 2009). "Continuous dose-response relationship of the LDL-cholesterol-lowering effect of phytosterol intake". J Nutr 139 (2): 271–84. doi:10.3945/jn.108.095125. PMID 19091798.
- ↑ Weingärtner O. et al; Bohm, M.; Laufs, U. (2009). "Controversial role of plant sterol esters in the management of hypercholesterolaemia". European Heart Journal 30 (4): 404–9. doi:10.1093/eurheartj/ehn580. PMC 2642922. PMID 19158117.
- ↑ Carrol, Margaret (April 2012). "Total and High-density Lipoprotein Cholesterol in Adults: National Health and Nutrition Examination Survey, 2009–2010". CDC.
| ||||||||||||||||||||||||