Thrombus


A thrombus (Greek: θρόμβος), or blood clot, is the final product of the blood coagulation step in hemostasis. It is achieved via the aggregation of platelets that form a platelet plug, and the activation of the humoral coagulation system (i.e. clotting factors). A thrombus is normal in cases of injury, but pathologic in instances of thrombosis.
Mural thrombi are thrombi adherent to the vessel wall. They are not occlusive and affect large vessels, such as heart and aorta. Grossly they appear grey-red with alternating light and dark lines (lines of Zahn) which represent bands of fibrin (lighter) with entrapped white blood cells and red blood cells (darker).
Pathophysiology
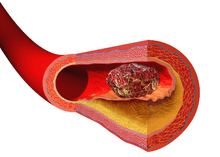
Specifically, a thrombus is the inappropriate activation of the hemostatic process in an uninjured or slightly injured vessel. A thrombus in a large blood vessel will decrease blood flow through that vessel (termed a mural thrombus). In a small blood vessel, blood flow may be completely cut-off (termed an occlusive thrombus) resulting in death of tissue supplied by that vessel. If a thrombus dislodges and becomes free-floating, it is termed as an embolus.
Some of the conditions which elevate risk of blood clots developing include atrial fibrillation (a form of cardiac arrhythmia), heart valve replacement, a recent heart attack (also known as a myocardial infarction), extended periods of inactivity (see deep venous thrombosis), and genetic or disease-related deficiencies in the blood's clotting abilities.
Formation
Platelet activation can occur through different mechanisms such as a vessel wall breach that exposes collagen, or tissue factor encryption. The platelet activation causes a cascade of further platelet activation eventually causing the formation of the thrombus.[1] This process is regulated through thromboregulation.
Treatment
Blood clot prevention and treatment reduces the risk of stroke, heart attack and pulmonary embolism. Heparin and warfarin are often used to inhibit the formation and growth of existing thrombi; the former binds to and activates the enzyme inhibitor antithrombin III, while the latter inhibits vitamin K epoxide reductase, an enzyme needed to synthesize mature clotting factors.
Some treatments have been derived from bacteria. One drug is streptokinase, which is an enzyme secreted by several streptococcal bacteria. This drug is administered intravenously and can be used to dissolve blood clots in coronary vessels. However, streptokinase is nonspecific and can digest almost any protein, which can lead to many secondary problems. Another clot-dissolving enzyme that works faster and is more specific is called tissue plasminogen activator (tPA). This drug is made by transgenic bacteria and it converts plasminogen into the clot-dissolving enzyme plasmin.[2] There are also some anticoagulants that come from animals that work by dissolving fibrin. For example, Haementeria ghilianii, an Amazon leech, produces an enzyme called hementin from its salivary glands.[3] As of 2012, this enzyme has now been successfully produced by genetically engineered bacteria and administered to cardiac patients.
Ultrasound-accelerated thrombolysis
A recent multicenter randomized trial (DUET[4]) compared standard catheter-directed thrombolysis (CDT) versus ultrasound-accelerated thrombolysis (USAT, EKOS Corporation) for the treatment of acute peripheral arterial thrombotic occlusions. Results showed that, on average, patients treated with USAT were completed 12 hours sooner than those treated with standard CDT with no increase in "serious adverse events."[5] Plans are underway to commence the DUET II study, which will be a non-randomized trial using the EKOS system with an even lower hourly drug dose with an expectation of further reducing bleeding complications.
Recent studies
Recent research shows that chemicals found in certain foods as onions, apples and oranges could help prevent blood clots. Researchers claim that rutin found in black and green teas also could help prevent the formation of clots and therefore could help in future treatments to protect against strokes and heart attacks.[6]
Presentation
Virchow's triad describes the pathogenesis of thrombus formation:
- Endothelial injury (injury to the endothelial cells that line enclosed spaces of the body, such as the inside of blood vessels) (e.g. trauma, atheroma)
- Abnormal blood flow (loss of laminar flow resulting from stasis in veins or turbulence in arteries) (e.g. valvulitis, aneurysm)
- Hypercoagulability (e.g. leukaemia, Factor V mutation (Leiden))
Disseminated intravascular coagulation (DIC) involves widespread microthrombi formation throughout the majority of the blood vessels. This is due to excessive consumption of coagulation factors and subsequent activation of fibrinolysis using all of the body's available platelets and clotting factors. The end result is hemorrhaging and ischaemic necrosis of tissue/organs. Causes are septicaemia, acute leukaemia, shock, snake bites, fat emboli from broken bones, or other severe traumas. DIC may also be seen in pregnant females. Treatment involves the use of fresh frozen plasma to restore the level of clotting factors in the blood, platelets and heparin to prevent further thrombi formation.
Thoracic aortic thrombus is a rare pathology that usually originates from an atherosclerotic aortic wall lesion or an aortic aneurysm and is a potential source of visceral, cerebral and peripheral embolism.[7][8]
Prognosis
Thrombus formation can have one of four outcomes: propagation, embolization, dissolution, and organization and recanalization.[9]
- Propagation of a thrombus occurs towards the direction of the heart. This means that it is anterograde in veins or retrograde in arteries.
- Embolization occurs when the thrombus breaks free from the vascular wall and becomes mobile. A venous emboli (most likely from deep venous thrombosis in the lower extremities) will travel through the systemic circulation, reach the right side of the heart, and travel through the pulmonary artery resulting in a pulmonary embolism. On the other hand, arterial thrombosis resulting from hypertension or atherosclerosis can become mobile and the resulting emboli can occlude any artery or arteriole downstream of the thrombus formation. This means that cerebral stroke, myocardial infarction, or any other organ can be affected.
- Dissolution occurs when fibrinolytic mechanisms break up the thrombus and blood flow is restored to the vessel. This may be aided by drugs (for example after occlusion of a coronary artery). The best response to fibrinolytic drugs is within a couple of hours, before the fibrin meshwork of the thrombus has been fully developed.
- Organization and recanalization involves the ingrowth of smooth muscle cells, fibroblasts and endothelium into the fibrin-rich thrombus. If recanalization proceeds it provides capillary-sized channels through the thrombus for continuity of blood flow through the entire thrombus but may not restore sufficient blood flow for the metabolic needs of the downstream tissue.
See also
- Embolism
- Thrombolysis ("Destruction of clot")
- Thrombogenicity (the tendency to clot)
- National Blood Clot Alliance
- Prothrombin time
References
- ↑ Furie, Bruce; Furie, Barbara (2008). "Mechanisms of Thrombus Formation". The New England Journal of Medicine 359 (9). doi:10.1056/NEJMra0801082. PMID 18753650.
- ↑ Saladin, Kenneth S. (2012). Anatomy & Physiology: The Unity of Form and Function (6th ed.). New York, NY: McGraw-Hill. p. 710. ISBN 978-0-07-337825-1.
- ↑ Malinconico, S. M., J. B. Katz, and A. Z. Budzynski. "Hementin: Anticoagulant Protease from the Salivary Gland of the Leech Haementeria Ghilianii." National Center for Biotechnology Information. U.S. National Library of Medicine, n.d. Web. 11 Dec. 2012.
- ↑ Schrijver, AM; et al (2011). "Dutch randomized trial comparing standard catheter-directed thrombolysis versus ultrasound-accelerated thrombolysis for thromboembolic infrainguinal disease (DUET): design and rationale". Trials 12: 20. doi:10.1186/1745-6215-12-20. PMID 21255459.
- ↑ "Randomized Controlled Multi-Center Trial Demonstrates Reduced Treatment Time and Drug Dose with EKOS vs. Catheter-Directed Thrombolysis in Peripheral Arterial Occlusions". EKOS Corporation/Bothell, WA. www.ekoscorp.com. April 15, 2013. Retrieved April 19, 2013.
- ↑ Prescott, Bonnie. "Flavonoid compound can prevent blood clots". Harvard Gazette. Retrieved 27 May 2012.
- ↑ Fueglistaler, P; Wolff T, Guerke L, Stierli P, Eugster T (2005). "Endovascular stent graft for symptomatic mobile thrombus of the thoracic aorta". J Vasc Surg 42 (4): 781–783. doi:10.1016/j.jvs.2005.05.054. PMID 16242568.
- ↑ Ungprasert, P; Ratanapo S, Cheungpasitporn W. "Management in Thoracic Aorta Mural Thrombi: Evidence Based Medicine and Controversy". Emergency Medicine 1 (e104). doi:10.4172/2165-7548.1000e104.
- ↑ Kumar, Vinay; et al. (2007). Robbins Basic Pathology (8th ed.). Philadelphia: Saunders/Elsevier. ISBN 978-1-4160-2973-1.
External links
| Look up thrombus or clot in Wiktionary, the free dictionary. |
- Treatment and Symptoms of Blood Clots -- MDhealthnetwork.org, Medical Information Resource, 1999
- North American Thrombosis Forum - NATF is a nonprofit organization dedicated to promoting thrombosis research, prevention and education, public policy, and advocacy outreach.
- Muscle Relaxing Drugs Can Reduce Lethal Blood Clots
- Air Pollution Triggers Blood Clots - US Study.
- The National Alliance for Thrombosis and Thrombophilia - has extensive stories from patients and family members on living with Thrombosis and Thrombophilia, assembled frequently asked questions and created publications addressing specific blood clot issues.
| |||||||||||||||||||||||||||||||||||||||