White blood cell

White blood cells, or leukocytes, are cells of the immune system defending the body against both infectious disease and foreign materials. Five[1] different and diverse types of leukocytes exist, but they are all produced and derived from a multipotent cell in the bone marrow known as a hematopoietic stem cell. Leukocytes are found throughout the body, including the blood and lymphatic system.[2]
The number of leukocytes in the blood is often an indicator of disease. There are normally between 4×109 and 11×109 white blood cells in a litre of blood, making up approximately 1% of blood in a healthy adult.[3] In conditions such as leukemia, the number of leukocytes is higher than normal, and in leukopenia, this number is much lower. The physical properties of leukocytes, such as volume, conductivity, and granularity, may change due to activation, the presence of immature cells, or the presence of malignant leukocytes in leukemia.
Contents |
Etymology
The name "White blood cell" derives from the fact that after centrifugation of a blood sample, the white cells are found in the Buffy coat, a thin layer of nucleated cells between the sedimented red blood cells and the blood plasma, which is typically white in color. The scientific term leukocyte directly reflects this description, derived from Greek leukos - white, and kytos - cell. Blood plasma may sometimes be green if there are large amounts of neutrophils in the sample, due to the heme-containing enzyme myeloperoxidase that they produce.
Types
There are several different types of white blood cells. They all have many things in common, but are all different. One primary technique to classify them is to look for the presence of granules, which allows the differentiation of cells into the categories granulocytes and agranulocytes:
- Granulocytes (polymorphonuclear leukocytes): leukocytes characterised by the presence of differently staining granules in their cytoplasm when viewed under light microscopy. These granules are membrane-bound enzymes which primarily act in the digestion of endocytosed particles. There are three types of granulocytes: neutrophils, basophils, and eosinophils, which are named according to their staining properties.
- Agranulocytes (mononuclear leucocytes): leukocytes characterized by the apparent absence of granules in their cytoplasm. Although the name implies a lack of granules these cells do contain non-specific azurophilic granules, which are lysosomes[4]. The cells include lymphocytes, monocytes, and macrophages.[5]
Overview table
| Type | Microscopic Appearance | Diagram | Approx. % in adults[6] See also: Blood values |
Diameter (μm)[6] | Main targets[3] | Nucleus[3] | Granules[3] | Lifetime[6] |
|---|---|---|---|---|---|---|---|---|
| Neutrophil | 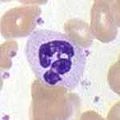 |
 |
54-62%[7] | 10-12 | multilobed | fine, faintly pink | 6 hours-few days (days in spleen and other tissue) |
|
| Eosinophil |  |
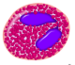 |
1-6% | 10-12 | bi-lobed | full of pink-orange (when stained) | 8-12 days (circulate for 4-5 hours) | |
| Basophil |  |
 |
<1% | 12-15 |
|
bi- or tri-lobed | large blue | ? |
| Lymphocyte | 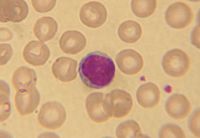 |
 |
25-33% | 7-8 | deeply staining, eccentric | NK-cells and Cytotoxic (CD8+) T-cells [8] | weeks to years | |
| Monocyte |  |
2-8% | 14-17 | Monocytes migrate from the bloodstream to other tissues and differentiate into tissue resident macrophages or dendritic cells. | kidney shaped | none | hours-days | |
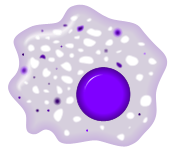
| Macrophage | 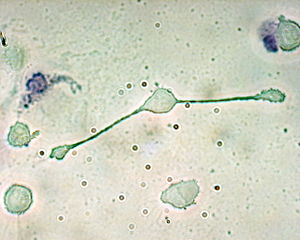 |
 |
21 (human)[9] 13 (rat)[10] | Phagocytosis (engulfment and digestion) of cellular debris and pathogens, and stimulation of lymphocytes and other immune cells that respond to the pathogen. | activated=days immature=months-years | |||
| Dendritic cells | 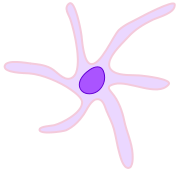 |
Main function is as an antigen-presenting cell (APC) that activates T lymphocytes. | similar to macrophages |
Neutrophil
Neutrophils defend against bacterial or fungal infection and other very small inflammatory processes that are usually first responders to microbial infection; their activity and death in large numbers forms pus. They are also known as polymorphonuclear leukocytes. They have a multilobed nucleus which may appear like multiple nuclei, hence the name polymorphonuclear leukocyte. The cytoplasm may look transparent because of fine granules that are faintly pink in color. Neutrophils are very active in phagocytosing bacteria and are present in large amount in the pus of wounds. These cells are not able to renew their lysosomes used in digesting microbes and die after having phagocytosed a few pathogens .
Eosinophil
Eosinophils primarily deal with parasitic infections and an increase in them may indicate such. Eosinophils are also the predominant inflammatory cells in allergic reactions. The most important causes of eosinophilia include allergies such as asthma, hay fever, and hives; and also parasitic infections. Generally their nucleus is bi-lobed. The cytoplasm is full of granules which assume a characteristic pink-orange color with eosin stain.
Basophil
Basophils are chiefly responsible for allergic and antigen response by releasing the chemical histamine causing inflammation. The nucleus is bi- or tri-lobed, but it is hard to see because of the number of coarse granules which hide it. They are characterised by their large blue granules.
Lymphocyte
Lymphocytes are much more common in the lymphatic system. Lymphocytes are distinguished by having a deeply staining nucleus which may be eccentric in location, and a relatively small amount of cytoplasm. The blood has three types of lymphocytes:
- B cells: B cells make antibodies that bind to pathogens to enable their destruction. (B cells not only make antibodies that bind to pathogens, but after an attack, some B cells will retain the ability to produce an antibody to serve as a 'memory' system.)
- T cells:
- CD4+ (helper) T cells co-ordinate the immune response and are important in the defense against intracellular bacteria. In acute HIV infection, these T cells are the main index to identify the individual's immune system activity. Research has shown [11] that CD8+ cells are also another index to identify human's immune activity.
- CD8+ cytotoxic T cells are able to kill virus-infected and tumor cells.
- γδ T cells possess an alternative T cell receptor as opposed to CD4+ and CD8+ αβ T cells and share characteristics of helper T cells, cytotoxic T cells and natural killer cells.
- Natural killer cells: Natural killer cells are able to kill cells of the body which are displaying a signal to kill them, as they have been infected by a virus or have become cancerous.
Monocyte
Monocytes share the "vacuum cleaner" (phagocytosis) function of neutrophils, but are much longer lived as they have an additional role: they present pieces of pathogens to T cells so that the pathogens may be recognized again and killed, or so that an antibody response may be mounted. Monocytes eventually leave the bloodstream to become tissue macrophages which remove dead cell debris as well as attacking microorganisms. Neither of these can be dealt with effectively by the neutrophils. Unlike neutrophils, monocytes are able to replace their lysosomal contents and are thought to have a much longer active life. They have the kidney shaped nucleus and are typically agranulated. They also possess abundant cytoplasm.
Macrophage
Once monocytes move from the bloodstream out into the body tissues, they undergo changes (differentiate) allowing phagocytosis and are then known as macrophages.
Medications causing leukopenia
Some medications can have an impact on the number and function of white blood cells. Leukopenia is the reduction in the number of white blood cells, which may affect the overall white cell count or one of the specific populations of white blood cells. For example, if the number of neutrophils is low, the condition is known as neutropenia. Likewise, low lymphocyte levels are termed lymphopenia. Medications which can cause leukopenia include clozapine, an antipsychotic medication with a rare adverse effect leading to the total absence of all granulocytes (neutrophils, basophils, eosinophils). Other medications include immunosuppressive drugs, such as sirolimus, mycophenolate mofetil, tacrolimus, and cyclosporine. Interferons used to treat multiple sclerosis, like Rebif, Avonex, and Betaseron, can also cause leukopenia.
White blood cells seen under the dark field microscope
White blood cells can be seen as live cells with the dark field microscope. This method allows judgement of the viability of the white blood cells, which is not possible with stained samples. [12]
Fixed leukocytes
Some leukocytes migrate into the tissues of the body to take up a permanent residence at that location rather than remaining in the blood. Often these cells have specific names depending upon which tissue they settle in, such as fixed macrophages in the liver which become known as Kupffer cells. These cells still serve a role in the immune system.
- Histiocytes
- Dendritic cells (Although these will often migrate to local lymph nodes upon ingesting antigens)
- Mast cells
- Microglia
References
- ↑ Brooks, Myrna LaFleur (2008). Exploring Medical Language: A Student-Directed Approach, 7th Edition. St. Louis, Missouri, USA: Mosby Elsevier. pp. 398. ISBN 978-0-323-04950-4.
- ↑ Maton, die; Jean Hopkins, Charles William McLaughlin, Susan Johnson, Maryanna Quon Warner, David LaHart, Jill D. Wright (1000008). Human Biology and Health. Englewood Cliffs, New Jersey, USA: Prentice Hall. ISBN 0-13-981176-1.
- ↑ 3.0 3.1 3.2 3.3 Alberts, Bruce (2005). "Leukocyte functions and percentage breakdown". Molecular Biology of the Cell. NCBI Bookshelf. Retrieved on 2007-04-14.
- ↑ Gartner, Leslie P.; Hiatt, James L. (2007). written at ,China. Color Textbook of Histology (3rd ed.). Philadelphia, PA: SAUNDERS Elsevier. pp. p. 225. ISBN 978-1-4160-2945-8.
- ↑ http://www.wisc-online.com/objects/index_tj.asp?objID=AP14704
- ↑ 6.0 6.1 6.2 Daniels, Victor G.; Wheater, Paul R.; Burkitt, H. George (1979). Functional histology: a text and colour atlas. Edinburgh: Churchill Livingstone. ISBN 0-443-01657-7.
- ↑ http://www.wisc-online.com/objects/index_tj.asp?objID=AP14704
- ↑ Semester 4 medical lectures at Uppsala University 2008 by Leif Jansson
- ↑ Environemental Health Perspectives 150(5), Sept. 1997
- ↑ Environmental Health Perspectives 150(5), Sept. 1997
- ↑ Pantaleo 1994
- ↑ http://www.darkfieldtraining.com/main/page_events__articles_lba_and_its_credibility.html
External links
|
||||||||||||||
|
|||||||||||||||||||||||