Plantar wart
| Plantar wart Classification and external resources |
|
 |
|
|---|---|
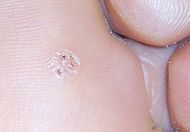
| A plantar wart. Striae (fingerprints) go around the lesion. | |
| ICD-10 | B07 |
| ICD-9 | 078.12 |
A plantar wart (also verruca plantaris or commonly known as verruca) is a wart caused by the human papillomavirus (HPV) occurring on the sole or toes of the foot. (HPV infections in other locations are not plantar; see human papillomavirus.) Plantar warts are usually self-limiting, but should be treated to lessen symptoms (which may include pain), decrease duration, and reduce transmission. [1]
Contents |
Infection and development
It is estimated that 7-10% of the US population is infected. Infection typically occurs on moist walking surfaces such as showers, swimming pools, or shoes. The virus can survive many months without a host, making it highly contagious.[1][2]
Plantar warts are benign epithelial tumors caused by infection by human papilloma virus types 1, 2, 4, or 63. These types are classified as clinical (visible symptoms). The virus attacks the skin through direct contact, entering through possibly tiny cuts and abrasions in the stratum corneum (outermost layer of skin). After infection, warts may not become visible for several weeks or months. Because of pressure on the sole of the foot, the wart is pushed inward and a layer of hard skin may form over the wart. A plantar wart can be painful if left untreated.[1][3]
Warts may spread through autoinoculation, by infecting nearby skin or by infecting walking surfaces. Plantar warts may also spread to other parts of the body.[4] They may fuse or develop into clusters called mosaic warts.[2]
Diagnosis
A plantar wart is a small lesion that appears on the sole of the foot and typically resembles a cauliflower, with tiny black petechiae (abnormal, thrombosed capillaries resembling specks) in the center. Pinpoint bleeding may occur when these are scratched, and they may be painful when standing or walking.[2][3]
Plantar warts are often similar to calluses or corns, but can be differentiated by close observation of skin striations. Feet are covered in skin striae, which are akin to fingerprints on the feet. Skin striae go around plantar warts; if the lesion is not a plantar wart, the cells' DNA is not altered and the striations continue across the top layer of the skin. Plantar warts tend to be painful on application of pressure from either side of the lesion rather than direct pressure, unlike calluses (which tend to be painful on direct pressure instead).
Prevention and treatment
Because plantar warts are spread by contact with moist walking surfaces, they can be prevented by not walking barefoot in public areas such as showers or communal changing rooms, not sharing shoes and socks, and avoiding direct contact with warts on other parts of the body or on other people. Humans build immunity with age, so infection is less common among adults than children.[3]
Once a person is infected, there is no evidence that any treatment eliminates HPV infection or decreases infectivity, and warts may recur after treatment because of activation of latent virus present in healthy skin adjacent to the lesion. There is currently no vaccine for these types of the virus. However, treatments are sometimes effective at addressing symptoms and causing remission (inactivity) of the virus.[2]
The treatment that will be effective in a particular case is highly variable. The most comprehensive medical review found that no treatment method was more than 73% effective and using a placebo had a 27% average success rate.[5]
Some treatments that have been found to be effective include:[6]
| First-line therapy | over the counter salicylic acid |
| Second-line therapy | Cryosurgery, intralesional immunotherapy, or pulsed dye laser therapy |
| Third-line therapy | Bleomycin, surgical excision |
Podiatrists and dermatologists are considered specialists in the treatment of plantar warts, though most warts are treated by primary care physicians.
As warts are contagious, precautions should be taken to avoid spreading.
Pharmaceutical treatments
- Keratolytic chemicals
- The treatment of warts by keratolysis involves the peeling away of dead surface skin cells with trichloroacetic acid or salicylic acid.
- Immunotherapy
- Intralesional injection of antigens (mumps, candida or trichophytin antigens USP) is a new wart treatment which may trigger a host immune response to the wart virus, resulting in wart resolution. Distant, non-injected warts may also disappear.
- Chemotherapy
- Topical application of dilute glutaraldehyde (a virucidal chemical, used for cold sterilization of surgical instruments) is an older effective wart treatment. More modern chemotherapy agents, like 5-fluoro-uracil, are also effective topically or injected intralesionally. Retinoids, systemically (eg. isotretinoin) or topically (tretinoin cream) may be effective.
Surgical
- Liquid nitrogen : Cryosurgery with liquid nitrogen. A common treatment that works by producing a blister under the wart. It is painful but usually nonscarring.
- Electrodesiccation and surgical excision produce scarring. If the wart recurs, the patient has a permanent scar along with the wart.
- Lasers may be effective, especially the 585nm pulsed dye laser which the most effective treatment of all, and does not leave scars, but is generally a last resort treatment as it is expensive and painful, and multiple laser treatments are required (generally 4-6 treatments repeated once a month until the wart disappears).
- Cauterization may be effective as a prolonged treatment. As a short-term treatment, cauterization of the base with anaesthetic can be effective but risks scars or keloids. Subsequent surgical removal is unnecessary, and risks keloids and recurrence in the operative scar.[7]
Other
- Watchful waiting is discouraged due to significantly increased likelihood of passing on the virus and the possibility that in some individuals the virus may spread more extensively over the skin surface, further increasing discomfort and making treatment more difficult and requiring it to be more extensive. However some warts eventually resolve due to the patient's own immune system. In many cases, the body will attack and kill the wart and verrucæ will turn black and effectively fall off, although it can be two years or longer before this takes place.
- Hyperthermia through the immersion of the wart in hot water (113°F or 45°C) for 30 minutes to 3 hours, 2–3 times per week, up to 16 treatments.[8][9]
Relative effectiveness of treatments
A 2006 study assessed the effects of different local treatments for cutaneous, non-genital warts in healthy people.[5] The study reviewed 60 randomized clinical trials dating up to March 2005. The main findings were:
- overall there is a lack of evidence (many trials were excluded because of poor methodology and reporting).
- the average cure rate using a placebo was 27% after an average period of 15 weeks.
- the best treatments are those containing salicylic acid. They are clearly better than placebo.
- there is surprisingly little evidence for the absolute efficacy of cryotherapy.
- two trials comparing salicylic acid and cryotherapy showed no significant difference in efficacy.
- one trial comparing salicylic acid and duct tape occlusion therapy showed no significant difference in efficacy.
- evidence for the efficacy of the remaining treatments was limited.
References
- ↑ 1.0 1.1 1.2 Warts, Plantar at eMedicine
- ↑ 2.0 2.1 2.2 2.3 Human Papillomavirus at eMedicine
- ↑ 3.0 3.1 3.2 "Understanding Plantar Warts". Health Plan of New York. Retrieved on 2007-12-07.
- ↑ MedlinePlus Encyclopedia [1]
- ↑ 5.0 5.1 Gibbs S, Harvey I, Sterling JC, Stark R (2001). "Local treatments for cutaneous warts". Cochrane Database Syst Rev (2): CD001781. doi:. PMID 11406008. http://www.cochrane.org/reviews/en/ab001781.html.
- ↑ Bacelieri R, Johnson SM (August 2005). "Cutaneous warts: an evidence-based approach to therapy". Am Fam Physician 72 (4): 647–52. PMID 16127954. http://www.aafp.org/afp/20050815/647.html.
- ↑ Kunnamo, Ilkka (2005). Evidence-based Medicine Guidelines. John Wiley and Sons. pp. 422. ISBN 9780470011843. http://books.google.ca/books?id=frYEiHYtOv0C&pg=PA422&lpg=PA422&ots=SKReQQJ28F&sig=nUlPPXUpfHJeO4-Rn-bmLyCDjfY.
- ↑ Warts, Nongenital at eMedicine
- ↑ "Warts, plantar". medFamily. Retrieved on 2008-08-07.
External links
|
||||||||||||||||||||||||||||||||||||