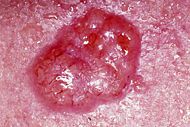
Basal cell carcinoma
| Basal cell carcinoma Classification and external resources |
|
 |
|
|---|---|
| ICD-9 | 173 |
| ICD-O: | 8090/3-8093/3 |
| OMIM | 605462 |
| DiseasesDB | 1264 |
| MedlinePlus | 000824 |
| eMedicine | med/214 |
| MeSH | D002280 |
Basal cell carcinoma is a type of skin cancer. It is the most common of all types of skin cancers. It is a malignant epithelial cell tumor that begins as a papule (a small, circumscribed, solid elevation of the skin) and enlarges peripherally, developing into a crater that erodes, crusts and bleeds. Metastasis is rare, but local invasion destroys underlying and adjacent tissue. In 90 percent of all cases, the lesion is seen between the hairline and the upper lip. It can be destructive and disfiguring. The risk of skin cancer is related to the amount of sun exposure and pigmentation in the skin. The longer the exposure to the sun and the lighter the skin, the greater the risk of skin cancer. There are three types of BCC: The most common type of basal cell carcinoma is nodular basal cell carcinoma, a flesh-colored (cream to pink), round or oval translucent nodule with overlying small blood vessels and a pearly-appearing rolled border. The second type of BCC is the pigmented lesion. This is darker than the nodular type, appearing blue, brown or black. It may be similar in appearance to the very aggressive malignant melanoma tumor. It is very important to distinguish between malignant melanomas and pigmented BCC. A third type of BCC is the superficial type, which appears as red, and often scaly, localized plaque. It is frequently confused with psoriasis or eczema. Basal cell skin cancer almost never spreads; however, large and longstanding tumours may metastasize into regional lymph nodes and surrounding areas such as nearby tissues and bone.[1][2]
Contents |
Forms
Various forms are recognized:
- Nodular: flesh-colored papule with telangiectasis; if it ulcerates, it becomes a "rodent ulcer" (ulcus rodens), an ulcerating nodule with (often) a pearly border
- Cystic: rarer and difficult to distinguish from the nodular form, which has a central cavity with fluid
- Pigmented: a variant of the nodular form that may be confused with melanoma
- Sclerosing/cicatrizing or Morpheaform: a scar-like lesion. Also called "infiltrative".
- Superficial: a red scaling patch.
- Basal cell cancer with squamous differentiation: Or Baso-squamoid variant. Often consider to be more agressive, and should be treated with respect especially when found on the ears, lips, or in immunosuppressed individuals. Probably is responsible for the reported deaths and metastasis. It behaves more like a squamous cell carcinoma than a basal cell cancer.
About two-thirds of basal cell carcinomas occur on sun-exposed areas of the body. One-third occur on areas of the body that are not exposed to sunlight, emphasizing the genetic susceptibility of the basal cell cancer patients.
Presentation
Basal cell carcinomas present as a firm nodule, clearly growing within the skin and below it, rather than on the surface.
Color varies from that of normal skin to dark brown or black, but there is a characteristic "pearly white" translucent quality on the periphery.
Basal cell carcinomas display a characteristic "rolled edge." Once the basal cells have invaded the deeper tissues, the rolled edge disappears.
When BCCs occur at sites other than the face and neck, they are usually just red, flat, scaling areas. Thus, superficial BCCs can often be confused with a patch of eczema.
Diagnosis
To diagnose basal cell carcinomas, a skin biopsy (where tissue is taken for pathological study) is done using local anesthesia. A suspected basal cell cancer should be biopsied first, and the final surgery is performed after the initial diagnosis is confirmed. The standard surgical margin for basal cell carcinoma (4 to 6 mm) is excessive to allow simple excisional biopsy to be performed even for small basal cell carcinoma. In rare cases, amelanotic melanoma and metastatic carcinoma can mimic basal cell cancers.
Histopathology: Basal cell carcinoma is a malignant epithelial tumor arising only in skin, from the basal layer of the epidermis or of the pilosebaceous adnexa. Tumor is represented by compact areas, well delineated and invading the dermis, apparently with no connection with the epidermis. Tumor cells resemble normal basal cells (small, monomorphous) and are disposed in palisade at the periphery of the tumor nests, but are spindle-shaped and irregular in the middle. Tumor clusters are separated by a reduced stroma with inflammatory infiltrate. 1
Pathophysiology

Basal cell carcinomas develop in the basal cell layer of the skin. Sun light exposure leads to the formation of thymine dimers, a form of DNA damage. While DNA repair removes most UV-induced damage, not all crosslinks are excised. There is, therefore, cumulative DNA damage leading to mutations. Apart from the mutagenesis, sunlight depresses the local immune system, possibly decreasing immune surveillance for new tumor cells.
Basal-cell carcinoma also develops as a result of basal-cell nevus syndrome, or Gorlin's syndrome, which is also characterized by odontogenic keratocysts of the jaw, palmar or plantar (sole of the foot) pits, calcification of the falx cerebri (in the center line of the brain) and rib abnormalities. The cause of the syndrome is a mutation in the PTCH1 tumor-suppressor gene at chromosome 9q22.3, which inhibits the hedgehog signaling pathway. A mutation in the SMO gene, which is also on the hedgehog pathway, also causes basal-cell carcinoma.[3]
Prevention and early diagnosis
Basal cell carcinoma is the most common skin cancer. It occurs mainly in fair-skinned patients with a family history of this cancer. Sunlight is a factor in about two-thirds of these cancers, but one-third occur in non-sun-exposed areas. Therefore, doctors recommend sun screens.
The use of a chemotherapeutic agent such as 5-Fluorouracil or Imiquimod, can prevent development of skin cancer. It is usually recommended to individuals with extensive sun damage, history of multiple skin cancers, or precancerous growths. It is often repeated every 2 to 3 years to further decrease the risk of skin cancer.
Treatment
The following methods are employed in the treatment of basal cell carcinoma (BCC):
- Mohs surgery: Mohs surgery (or Mohs micrographic surgery) is an outpatient procedure in which the tumor is surgically excised and then immediately examined under a microscope. It is often claimed to have the highest cure rate of 97% to 99.8% by some individuals. The base and edges are microscopically examined to verify sufficient margins before the surgical repair of the site. If the margins are insufficient, more is removed from the patient until the margins are sufficient. It is also used for squamous cell carcinoma; however, the cure rate is not as high as Mohs surgery for basal cell carcinoma.
- Chemotherapy: Some superficial cancers respond to local therapy with 5-fluorouracil, a chemotherapy agent. Topical treatment with 5% Imiquimod cream, with five applications per week for six weeks has a reported 70-90% success rate at reducing, even removing, the BCC [basal cell carcinoma]. Both Imiquimod and 5-fluorouracil has received FDA approval for the treatment of superficial basal cell carcinoma. Off label use of imiquimod on invasive basal cell carcinoma has been reported. Imiquimod may be used prior to surgery in order to reduce the size of the carcinoma. One can expect a great deal of inflammation with this treatment[4]. Chemotherapy often follows Mohs surgery to eliminate the residual superficial basal cell carcinoma after the invasive portion is removed. Removing the residual superficial tumor with surgery alone can result in large and difficult to repair surgical defects. One often waits a month or more after surgery before starting the Imiquimod or 5-fluorouracil to make sure the surgical wound has adequately healed. Some individual advocate the use of curettage (see EDC below) first, then followed by chemotherapy. These experimental procedure likely will result in better cure rate than one alone, but is not standard of care.
- Immunotherapy: Immunotherapy research suggests that treatment using Euphorbia peplus, a common garden weed, may be effective[5]. Australian biopharmaceutical company Peplin[6] is developing this as topical treatment for BCC. Imiquimod or Aldara is an immunotherapy but is listed here under chemotherapy.
- Radiation: Radiation therapy is appropriate for all forms of BCC as adequate doses will eradicate the disease. Although radiotherapy is generally used in older patients who are not candidates for surgery, it is also used in cases where surgical excision will be disfiguring or difficult to reconstruct (especially on the tip of the nose, and the nostril rims). The use of radiotherapy below the elbows and knees is not recommended as the blood supply to these areas is more easily affected by the radiation. Radiation treatment often takes as few as 5 visit to as many as 25 visits for radiation therapy. Usually, the more visits scheduled for therapy, the less complication or damage is done to the normal tissue supporting the tumor. Cure rate can be as high as 95% for small tumor, or as low as 80% for large tumors. Usually, recurrent tumors after radiation are treated with surgery, and not with radiation. Further radiation treatment will further damage normal tissue, and the tumor might be resistance to further radiation.
- Photodynamic Therapy: Photodynamic therapy is a new modality for treatment of basal-cell carcinoma, which is administrated by application of photosensitizers to the target area. When these molecules are activated by light, they become toxic, therefore destroy the target cells. Methyl aminolevulinate is approved by EU as a photosensitizer since 2001. This therapy is also used in other skin cancer types[7].
- Cryosurgery: Cryosurgery is an old modality for the treatment of many skin cancers. When accurately utilized with a temperature probe and a cryotherapy instruments, it can result in very good cure rate. Disadvantage is lack of margin control, tissue necrosis, over or under treatment of the tumor, and long recovery time. Several textbooks are published on the therapy, and a few physicians still apply the treatment to selected patients.
- Electrodessication and curettage: or EDC. One utilize a round knife, or curette, to scrape away the soft cancer. The next step is to burn the skin with an electric current. This further soften the skin, allowing for the knife to cut more deeply with the next layer of curettage. The cycle is repeated, with a safety margin of curettage of normal skin around the visible tumor. This cycle is repeated 3 to 5 times, and the free skin margin treated is usually 4 to 6 mm. Cure rate is very much user dependent and depends on the size and type of tumor. Infiltrative or morpheaform BCC's can be difficult to eradicate with EDC. Reserved only for non cosmetically important areas like the trunk. Some physicians believe that it is acceptable to utilize EDC on the face of elderly patients over the age of 70. However, with increasing life expectancy, such an objective criteria can not be supported. The cure rate can be low or high, depending on the aggressiveness of the EDC and the free margin treated.
- Standard surgical excision with either frozen section histology, or fixed tissue pathology. The cure rate for this method, whether done by a plastic surgeon, family doctor, or dermatologist is totally dependent on the surgical margin. A dermatoscope dermatoscopy can help an experienced surgeon accurately identify the visible tumor that the naked eye can not see. The narrower the free margin (skin removed that is free of visible tumor) the higher the recurrence rate. With special margin controlled processing and frozen section histology, a surgeon can assure a high cure rate approaching Mohs surgery. However, most standard excisions done in a plastic surgeon or dermatologist's office are sent to an outside laboratory for standard bread loafing method of processing. This method has a high "false negative" cure rate, due to the random sampling of the tumor. It is likely that less than 5% of the surgical margin is examined, as each slice of tissue is only 6 micron thick, and only about 3 to 4 sections are obtained. Usually, the rule of thumb is if a 4 mm free margin is obtained around a small tumor (less than 6mm), or a wider 6 mm free margin is obtained around a larger tumor (greater than 6mm), the cure rate is very high - 95% or better. Unfortunately, for cosmetic reasons, many doctors take only very small surgical margins 1-2 mm, especially when facial tumor is being removed. A pathology report from such a case indicating "margins free of residual tumor", often is inaccurate, and a high recurrence rate of up to 50% might occur. When in doubt, a patient should demand that either Mohs surgery or frozen section histology is utilized when dealing with a tumor on the face. The pathologist processing the frozen section specimen should cut multiple sections through the block to minimize the false negative error rate. Or one should simply process the tissue utilizing a method approximating the Mohs method (described in most basic histopathology text books) during frozen section processing. Unfortunately, these methods are difficult when applied to frozen sections; and is very tedious to process. When not utilizing frozen section, the surgeon will have to wait a week or more, before informing the patient if more tumor is left, or if the surgical margin is too narrow. And a second surgery must be performed to remove the residual or potential residual tumor.
Treating surgeons will recommend one of these modalities as appropriate treatment depending on the tumor size, location, patient age, and other variables.
Prognosis
Although basal cell carcinoma rarely metastasizes, it grows locally with invasion and destruction of local tissues, without stopping. The cancer can impinge on vital structures and result in loss of extension or loss of function or rarely death. The vast majority of cases can be successfully treated before serious complications occur. The recurrence rate for the above treatment options ranges from 50% to 1% or less.
In chosing the therapy, one must weights the benefit gained from the morbidity of the procedure. As most basal cell carciomas are slow growing, and not deadly; the health and age of the patient must be considered. Although difficult to discuss, radiation therapy, topical chemotherapy, or no treatment at all should be considered in ill or frail individuals in difficult to excise tumor of no immediate harm to the individual. While methods with the highest cure rate should be considered for young and healthy individuals with long life expectancy. It is here that one should seriously consider the cure rate of Mohs surgery vs. standard excision by a plastic surgeon vs. radiation therapy.
Epidemiology
Basal cell cancer is the most common skin cancer. It is much more common in fair-skinned individuals with a family history of basal cell cancer and increases in incidence closer to the equator or at higher altitude. According to Skin Cancer Foundation, there are approximately 800,000[8] new cases yearly in the United States alone.
Most sporadic BCC arises in small numbers on sun-exposed skin of people over age 50, although younger people may also be affected. The development of multiple basal cell cancer at an early age could be indicative of Nevoid basal cell carcinoma syndrome.
Notes
- ↑ MedlinePlus Encyclopedia Basal cell carcinoma
- ↑ "Basal Cell Carcinoma - Symptoms, Treatment and Prevention".
- ↑ Epstein EH, Shepard JA, Flotte TJ (Jan 2008). "Case records of the Massachusetts General Hospital. Case 3-2008. An 80-year-old woman with cutaneous basal-cell carcinomas and cysts of the jaws". N Engl J Med 358 (4): 393–401. doi:. PMID 18216361.
- ↑ The Skin Cancer Foundation - The Skin Cancer Foundation Seal of Recommendation
- ↑ Peplin's skin cancer gel trial a success - Breaking News - Business - Breaking News
- ↑ Peplin
- ↑ Peng Q et al (Jan 2008) "Lasers in Medicine" Rep. Prog. Phys. 71 056701
- ↑ Skin Cancer Foundation: Basal Cell Carcinoma
References
- "ACS :: Treating Basal Cell Carcinoma".
- Smeets NW, Krekels GA, Ostertag JU, et al (2004). "Surgical excision vs Mohs' micrographic surgery for basal-cell carcinoma of the face: randomised controlled trial". Lancet 364 (9447): 1766–72. doi:. PMID 15541449.
External links
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||
|
||||||||||||||